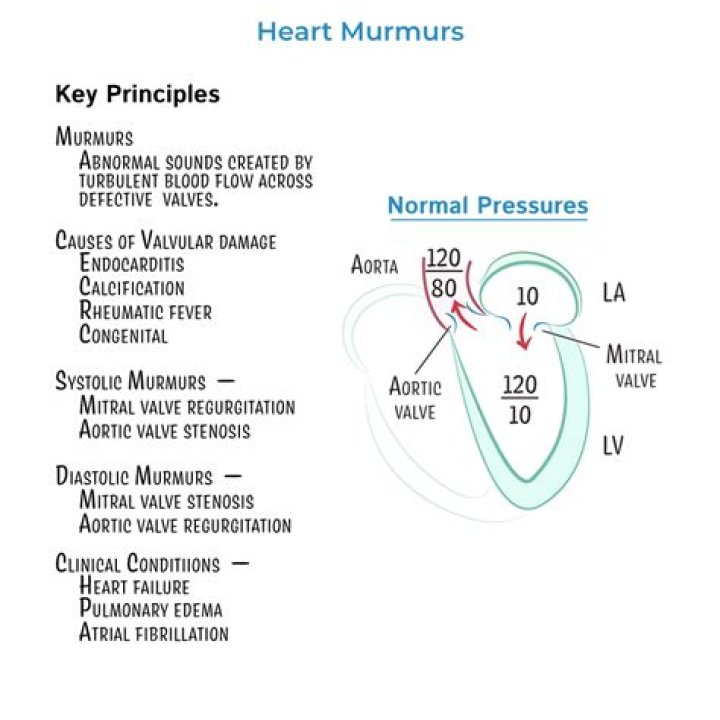
Can FFP cause transfusion reaction
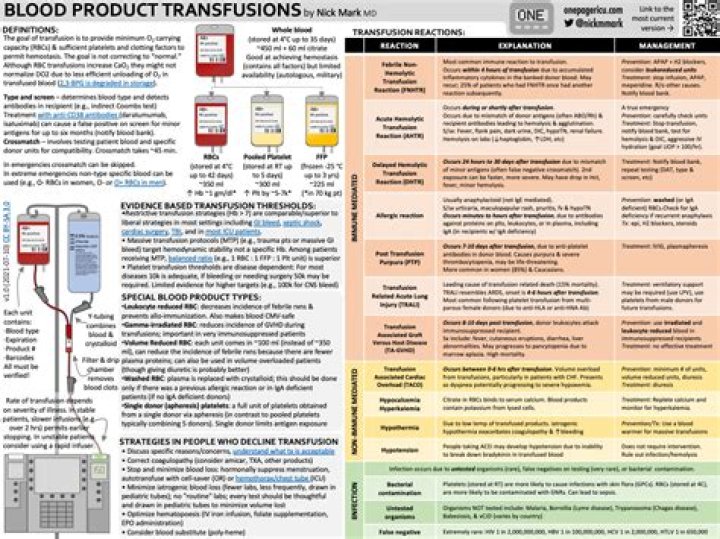

Allergic/anaphylactic reactions are commonly associated with FFP and platelet transfusions,87 and the rate of ATR to FFP found in two retrospective studies was 1:591 and 1:2,184 plasma units transfused.
Can you transfuse blood and FFP at the same time?
Yes, unless otherwise stated in the instructions for use on the blood tubing packaging you can transfuse red blood cells, platelets, plasma or cryo through the same filter set.
Does fresh frozen plasma contain red blood cells?
Fresh frozen plasma (FFP): This is platelet-poor plasma that is separated from red cells within 6 hours of blood collection and frozen in a dedicated freezer (at or below -20°C).
What are the potential causes of transfusion reaction?
What causes the transfusion reaction? Antibodies in the recipient’s blood can attack the donor blood if the two are not compatible. If the recipient’s immune system attacks the red blood cells of the donor, it is called a hemolytic reaction. You can have an allergic reaction to a blood transfusion as well.What is the most common cause of a blood transfusion reaction?
Cause: The majority of haemolytic reactions are caused by transfusion of ABO incompatible blood, eg group A, B or AB red cells to a group O patient.
Does blood type matter with FFP?
Plasma compatibility Plasma components (e.g. fresh frozen plasma, cryoprecipitate and cryodepleted plasma) should be compatible with the ABO group of the recipient to avoid potential haemolysis caused by donor anti-A or anti-B. Plasma components of any RhD type can be given regardless to the RhD type of the recipient.
Does FFP require cross matching?
FFP transfusions must be ABO compatible, but Rh compatibility and cross-matching are not required (Table 35.1).
What type of hypersensitivity is blood transfusion reaction?
Type II hypersensitivity is typified by a transfusion reaction in which mismatched red blood cells are rapidly destroyed by specific preformed antibodies (anti-ABO or -Rh) and complement.What can cause acute hemolytic transfusion reaction?
The most common cause of acute hemolytic transfusion reaction is ABO incompatibility, which is typically due to human error that results in a recipient receiving the incorrect blood product. Rarely, other blood type incompatibilities can cause AHTR, the most common of which is Kidd antigen incompatibility.
What is the number one cause of death associated with transfusions?Transfusion-related circulatory overload (TACO) remains the most common cause of transfusion-related death, although deaths due to delays are increasing year-on-year, shows an analysis of reports to the UK’s transfusion safety body.
Article first time published onIs FFP used for elevated PT PTT?
In general, FFP should be transfused when clotting studies become abnormal, including a prolonged prothrombin time (PT) or activated partial thromboplastin time (aPTT). Nonsurgical bleeding in children who receive more than 1 blood volume of PRBCs frequently require FFP due to factor V and VIII deficiency.
What is the difference between FFP and platelets?
Fresh frozen plasma infusion can be used for reversal of anticoagulant effects. Platelet transfusion is indicated to prevent hemorrhage in patients with thrombocytopenia or platelet function defects.
Why fresh frozen plasma is given?
Fresh frozen plasma is indicated for the deficiency of coagulation factors with abnormal coagulation tests in the presence of active bleeding.
When do blood transfusion reactions occur?
Reactions can occur between 1 day and 4 weeks after the transfusion. A person can acquire these antibodies through previous pregnancies or transfusions. These particular antibodies decrease over time to undetectable levels. Those with the antibodies have a higher chance of developing these transfusion reactions.
When do most blood transfusion reactions occur?
Acute transfusion reactions present as adverse signs or symptoms during or within 24 hours of a blood transfusion. The most frequent reactions are fever, chills, pruritus, or urticaria, which typically resolve promptly without specific treatment or complications.
How do you control a blood transfusion reaction?
- Antihistamines.
- Analgesics and Antipyretics.
- Osmotic Diuretics.
- Vasopressors.
- Loop Diuretics.
- Show All.
How do you transfuse FFP?
Methods of use. FFP must be thawed between 30 °C and 37 °C in a water bath under continuous agitation or with another system able to ensure a controlled temperature. The plasma must be transfused as soon as possible after thawing, but in any case within 24 hours, if stored at 4 ± 2 °C 4,5.
How does a person's blood type related to transfusion compatibility?
In the context of blood transfusions, a blood match is a compatibility between the donor’s blood and the recipient’s blood. This does not always mean an identical blood match. Red blood cells from a donor that is type O+ can be transfused into patients of four different blood types: A+, B+, AB+, and of course O+.
Why should blood be cross matched before transfusion?
The purpose of the crossmatch is to detect the presence of antibodies in the recipient against the red blood cells of the donor. These antibodies attach to the red blood cells of the donor after transfusion. An incompatible transfusion can result in a severe hemolytic anemia and even death.
What happens if Rh-negative receive Rh positive blood?
This is because an Rh-positive blood transfusion can cause a person with Rh negative blood to make antibodies against the Rh factor, causing a transfusion reaction (discussed below). If an Rh-negative woman makes antibodies like this, it can seriously harm any Rh-positive babies she may have in the future.
Can Rh-negative receive Rh positive plasma?
This protein is also often called the D antigen. When it comes to blood transfusion, anyone who is Rh positive can receive blood from someone who is Rh negative, but those with negative blood types cannot receive from anyone with a positive blood type.
What happens when a patient of blood group A gets a unit of O red blood cells?
If ABO incompatible red cells are transfused, red cell haemolysis can occur. For example if group A red cells are infused into a recipient who is group O, the recipient’s anti-A antibodies bind to the transfused cells.
What causes a hemolytic reaction?
A hemolytic transfusion reaction is a serious complication that can occur after a blood transfusion. The reaction occurs when the red blood cells that were given during the transfusion are destroyed by the person’s immune system. When red blood cells are destroyed, the process is called hemolysis.
Which of the following transfusion is likely to cause intravascular hemolysis?
Acute HTRs: These are due to preformed antibodies against donor RBC antigens present in the recipient’s blood. ABO incompatibility reactions are the most dreaded hemolytic transfusion reactions due to their ability to cause intravascular hemolysis.
How does intravascular hemolysis occur?
Intravascular hemolysis is the state when the red blood cell ruptures as a result of the complex of complement autoantibodies attached (fixed) on the surfaces of RBCs attack and rupture RBCs’ membranes, or a parasite such as Babesia exits the cell that ruptures the RBC’s membrane as it goes.
What type of hypersensitivity occurs when a patient receives the wrong blood type during a transfusion leading to a hemolytic transfusion reaction?
A transfusion with an incompatible ABO blood type may lead to a strong, potentially lethal type II hypersensitivity cytotoxic response called hemolytic transfusion reaction (HTR).
How do you prevent a reaction to a blood transfusion?
The most common approach to preventing FNHTR and allergic reactions is to give the patient premedication with an antipyretic such as paracetamol and an anti-histamine such as diphenydramine. There is very widespread use of these drugs prior to a transfusion.
What causes a Type II hypersensitivity reaction that is result of ABO mismatched blood transfusion?
In the case of Rh factor antigens, TH2 cells stimulate class switching to IgG, and this has important implications for the mechanism of HDN. Like ABO incompatibilities, blood transfusions from a donor with the wrong Rh factor antigens can cause a type II hypersensitivity HTR.
What is the biggest risk of transfusion?
Infections. In the past, infections were the biggest risk of blood transfusions. But because of today’s screening and prevention procedures, infections from blood transfusions are very rare. The chances of getting an infection from a blood transfusion in the United States are very low.
What transfusion reactions are the 3 most commonly reported causes of transfusion related mortality?
Today, the leading causes of allogeneic blood transfusion (ABT)–related mortality in the United States—in the order of reported number of deaths—are transfusion-related acute lung injury (TRALI), ABO and non-ABO hemolytic transfusion reactions (HTRs), and transfusion-associated sepsis (TAS).
Are transfusion reactions fatal?
Most transfusion reactions are not harmful. However, some, such as anaphylactic reactions, can be fatal. Transfusion should be stopped immediately when a reaction starts and the recipient should be monitored in case of more reactions.