How do you prevent a febrile transfusion reaction
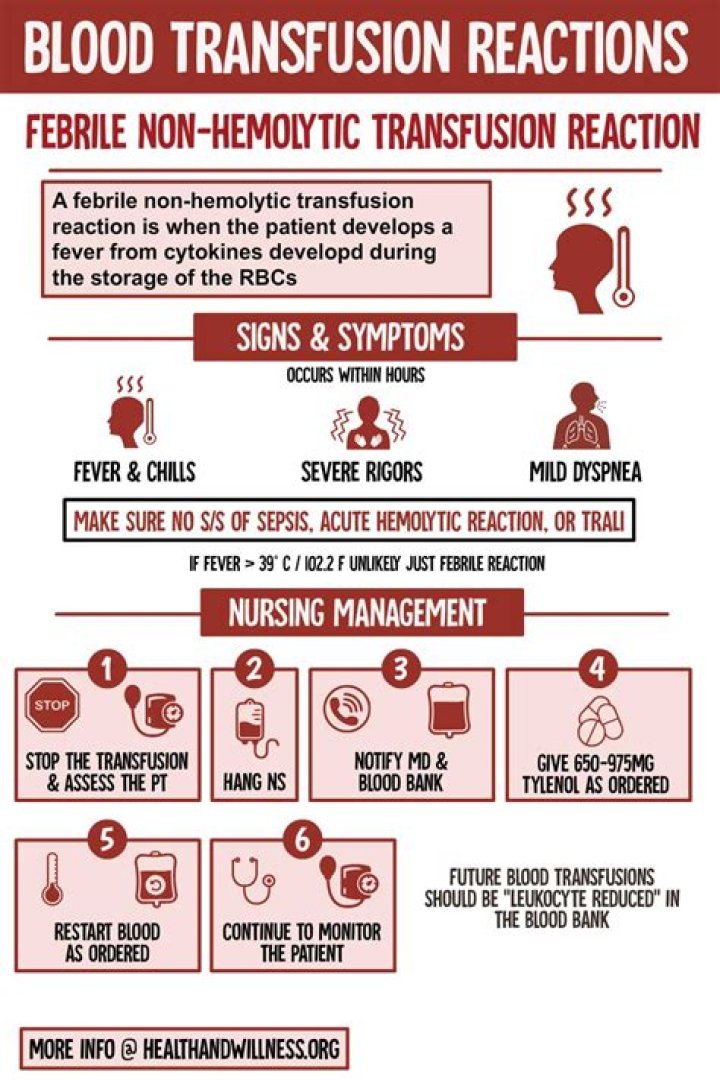
The best way to prevent severe febrile reactions is to use prestorage leukocyte reduced red blood cells and apheresis platelets. If a patient continues to have febrile reactions to leukocyte reduced single donor platelets, it may be helpful to remove plasma from the platelet unit immediately prior to transfusion.
How do you prevent a febrile Nonhemolytic transfusion reaction?
- PMID: 9372039.
- DOI: 10.1097/00062752-199502060-00013.
How do you stop a blood transfusion reaction?
The most common approach to preventing FNHTR and allergic reactions is to give the patient premedication with an antipyretic such as paracetamol and an anti-histamine such as diphenydramine. There is very widespread use of these drugs prior to a transfusion.
What practice can help reduce the number of febrile transfusion reactions?
Premedication with acetaminophen and diphenhydramine is the most commonly used approach to reduce the incidence of FNHTR and allergic reactions to blood products; it is used in 50% to 80% of transfusions in the US and Canada.What causes a febrile transfusion reaction?
Nonhemolytic febrile transfusion reactions are usually caused by cytokines from leukocytes in transfused red cell or platelet components, causing fever, chills, or rigors. In the transfusion setting, a fever is defined as a temperature elevation of 1º C or 2º F.
How does blood transfusion prevent hemolysis?
Prevention. Donated blood is put into ABO and Rh groups to reduce the risk for transfusion reaction. Before a transfusion, recipient and donor blood are tested (cross-matched) to see if they are compatible.
What causes febrile Nonhemolytic transfusion reaction?
Most febrile nonhemolytic transfusion reactions (FNHTR) to platelets are caused by cytokines that accumulate in the product during storage. There have been numerous studies that have demonstrated high concentrations of leukocyte- and platelet-derived cytokines in stored platelet products.
What follow up blood work may be required after a transfusion reaction?
In acute hemolytic reactions, the workup includes the following: Visual inspection of the recipient’s plasma and urine. Retyping of donor and recipient red blood cells (RBCs) Direct antiglobulin (Coombs) testing.Which product can help ease symptoms of an allergic transfusion reaction?
Diphenhydramine hydrochloride (Benadryl, Diphen) Among other indications, used to treat urticaria, pruritus, and other histamine-mediated manifestations of allergic reactions to blood products.
Who is at risk for febrile non hemolytic transfusion reaction?FNHTRs are more common in the transfusion of platelets. Multiply-transfused patients and multiparous women make up the largest populations experiencing this type of reaction. There are two mechanisms involved in the manifestation of an FNHTR.
Article first time published onWhat does Nonhemolytic mean?
Definition of nonhemolytic medical. : not causing or characterized by hemolysis : not hemolytic a nonhemolytic streptococcus.
What precautions should be taken before blood transfusion?
Before your transfusion, your nurse will: Check your blood pressure, pulse and temperature. Make sure the donor blood type is a match for your blood type.
What is a febrile reaction to blood transfusion?
Febrile reactions Cause: Fever and chills during transfusion are thought to be caused by recipient antibodies reacting with white cell antigens or white cell fragments in the blood product or due to cytokines which accumulate in the blood product during storage.
How can you prevent bacterial contamination of a blood product?
Using approved products and procedures, blood collection centers can implement practices that may decrease bacterial contamination, including better skin disinfection, collection of blood with a diversion pouch set, testing for bacteria, and, potentially, the use of safe and effective pathogen reduction technologies if …
What helps itching during blood transfusion?
Some people have allergic reactions to blood received during a transfusion, even when given the right blood type. In these cases symptoms include hives and itching. Like most allergic reactions, this can be treated with antihistamines. However, a doctor should be consulted if the reaction becomes serious.
Can you take Tylenol after a blood transfusion?
Reactions you can treat at home: (Tylenol) unless you are allergic to this or a history of problems with acetaminophen. Follow the directions on the package. If you have a rash, hives or itching, take an antihistamine medication such as Benadryl or Reactine. Follow the directions on the package.
Can you give medications during blood transfusion?
No medications may be added to blood units or through IV tubing. Specific blood administration tubing is required for all blood transfusions. Blood tubing is changed every 4 hours or 4 units, whichever comes first.
How do you assess a transfusion reaction?
The most common signs and symptoms include fever, chills, urticaria (hives), and itching. Some symptoms resolve with little or no treatment. However, respiratory distress, high fever, hypotension (low blood pressure), and red urine (hemoglobinuria) can indicate a more serious reaction.
Why is normal saline given after a blood transfusion reaction?
Background: It is standard practice at many hospitals to follow blood component transfusions with a normal saline (0.9% NaCl) flush. This serves the dual purpose of administering to the patient any residual blood left in the administration set (up to 40 mL), and it flushes the line for later use.
What is the first step in the investigation of a transfusion reaction?
Transfusion reactions require immediate recognition, laboratory investigation, and clinical management. If a transfusion reaction is suspected during blood administration, the safest practice is to stop the transfusion and keep the intravenous line open with 0.9% sodium chloride (normal saline).
What is a febrile non hemolytic reaction?
Febrile nonhemolytic transfusion reactions (FNHTRs) are common, occurring with 1–3% of transfusions. FNHTR manifests as fever and/or chills without hemolysis occurring in the patient during or within 4 hours of transfusion cessation. Diagnosis is made by excluding other causes of fever.
What is the number one cause of death associated with transfusions?
Transfusion-related circulatory overload (TACO) remains the most common cause of transfusion-related death, although deaths due to delays are increasing year-on-year, shows an analysis of reports to the UK’s transfusion safety body.
How can a blood transfusion cause anaphylactic shock?
Allergic reactions occur when patients have antibodies that react with proteins in transfused blood components. Anaphylaxis occurs where an individual has previously been sensitised to an allergen present in the blood and, on re-exposure, releases immunoglobulin E (IgE) or IgG antibodies.
What is Trali transfusion reaction?
(TRALI) TRALI is an acute complication following blood transfusion that is characterized by severe shortness of breath, often associated with fever and low blood pressure. Although rare, it is one of the most common causes of transfusion- related death.
Why Alpha hemolysis is green?
Alpha hemolysis (α) is the reduction of the red blood cell hemoglobin to methemoglobin in the medium surrounding the colony. This causes a green or brown discoloration in the medium.
Can we drink water during blood transfusion?
There are also no restrictions on activities before or during the transfusion, as long as it doesn’t interfere with the IV if the line is already placed. After the first 15 minutes of the transfusion, you can eat and drink or work on your phone or laptop.
How do you handle platelets?
- Once dispensed, platelets shall be immediately transported directly to the RN or LIP requesting the component for transfusion.
- Must remain at room temperature.
- Never place inside a Blood Bank blood cooler for any reason.
Can you transfuse a febrile patient?
With physician approval, a transfusion may be administered to a febrile patient. However, if a patient is febrile, consideration should be given to postponement of the blood transfusion, since the fever may mask the development of a febrile reaction to the blood component itself.
Which blood component is most susceptible to bacterial contamination?
Summary. Bacterial contamination of blood components poses the most prevalent transfusion-transmitted infectious risk. Platelet concentrates (PCs) are the blood components most susceptible to bacterial contamination due to their storage conditions being amenable for bacterial growth.
What is the most common contaminant found in blood transfusion bags?
Results. 14 blood bags representing 17.5% grew isolates of various bacteria. Ten (10) of the 14 isolates were Gram positive cocci representing 71.42% making it the commonest contaminant. 50% of the gram positive cocci were identified to be coagulase negative staphylococci and 21.42% were Staphylococcus aureus.
How can microorganisms evade the immune response?
Bacteria are multifaceted in their methods used to escape immune detection. They employ tactics such as modulating their cell surfaces, releasing proteins to inhibit or degrade host immune factors, or even mimicking host molecules.



