How does po2 change with altitude

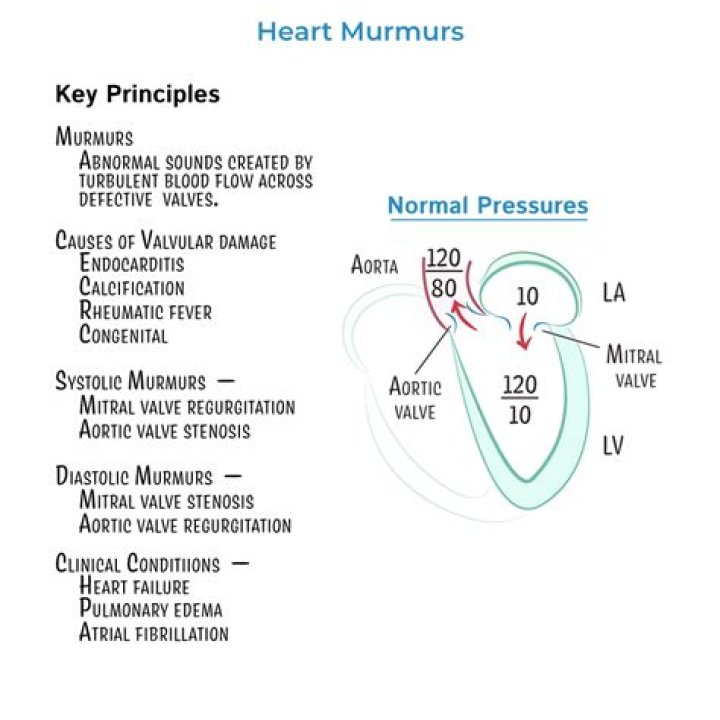
As the altitude increased the arterial PO2 decreased both at rest and for each given work level. On the “summit” where the inspired PO2 was 43 mmHg, the arterial PO2 was 30 mmHg at rest and this decreased to 28 mmHg at the maximal work rate of 120 watts.
What happens to pAO2 at high altitude?
Given that increasing altitude decreases the atmospheric pressure, for any given FiO2 you would expect a lower pAO2 and, consequently, a lower paO2. Conversely, increasing the barometric pressure can have significant effects by increasing the amount of dissolved oxygen. …
What happens when arterial PO2 decreases?
Decreased arterial PO2, not O2 content, increases blood flow through intrapulmonary arteriovenous anastomoses at rest.
How does altitude affect PCO2?
Hyperventilation at high altitude reduces the alveolar PCO2 by the increase in alveolar ventilation. Alveolar PO2 is thereby increased so that the alveolar- capillary driving gradient is partially preserved.How does CO2 change with altitude?
The volume percentage of CO2 in the air remains almost constant with increasing elevation (apart from local modifications near the ground). Consequently its partial pressure or concentration (mass per volume) decreases as the barometric pres- sure falls with increasing altitude.
How does high altitude affect blood gases?
At high altitude, there is less oxygen in the air that you breathe. This means that all of the blood from all areas of the lungs, is relatively short on oxygen or hypoxic. Unfortunately, the lungs still respond to the shortage of oxygen in the same way: by tightening the blood vessels.
Does arterial PO2 decrease with altitude?
As the altitude increased the arterial PO2 decreased both at rest and for each given work level. On the “summit” where the inspired PO2 was 43 mmHg, the arterial PO2 was 30 mmHg at rest and this decreased to 28 mmHg at the maximal work rate of 120 watts.
What happens to PO2 during hyperventilation?
The PO2 in the blood of the veins and capillary beds of the cortex was calculated from the lifetimes. … During hyperventilation, which lowered arterial PCO2 and increased pH of the blood, the average PO2 decreased in proportion to the decrease in arterial PCO2.Why does high altitude cause respiratory alkalosis?
As the oxygen tension of inspired air falls with increasing altitude in normal subjects, hyperventilation ensues. This acute respiratory alkalosis, induces increased renal excretion of bicarbonate, returning the pH back to normal, giving rise to compensated respiratory alkalosis or chronic hypocapnia.
How does PO2 affect hemoglobin saturation?As the PO2 decreases, hemoglobin saturation will eventually fall rapidly, at a PO2 of 40 mmHg hemoglobin is 75% saturated. Meanwhile, at a PO2 of 25 mmHg, hemoglobin is 50% saturated. This level is referred to as P50, where 50% of heme groups of each hemoglobin have a molecule of oxygen bound.
Article first time published onWhat is the relationship between hemoglobin and PO2?
In this tutorial, we will discuss how the concentration of oxygen in the blood plasma (partial pressure of O2 or pO2) affects oxygen-hemoglobin (O2-Hb) saturation. As O2 enters the vial of blood, the plasma pO2 increases and more O2 binds with hemoglobin.
What altitude does CO2 stay at?
CO2 occurs naturally throughout Earth’s atmosphere and is the primary radiative cooling agent in the energy balance of the mesosphere (~50-90 km altitude) and thermosphere (>90 km). The same properties of CO2 that cause it to trap heat in the troposphere (<15 km) make it an efficient cooler at higher altitudes.
At what altitude is CO2 measured?
The measurements are made at six height levels on the tower, from 11 m to 396 m above the ground. Near the ground there is a very large diurnal cycle which decreases with altitude.
Which gas is lighter than air?
Neon is lighter than air (density 0.900 g/L at STP, average atomic mass 20.17 g/mol) and could lift a balloon. Like helium, it is non-flammable.
Does altitude affect pulse ox?
High altitudes can cause low oxygen saturation levels or desaturation of an individual’s blood. It happens because of low atmospheric pressure at high altitudes. Oxygen saturation levels refer to the extent hemoglobin is bound or saturated to oxygen.
How does altitude affect atmospheric pressure?
As altitude rises, air pressure drops. In other words, if the indicated altitude is high, the air pressure is low. … As altitude increases, the amount of gas molecules in the air decreases—the air becomes less dense than air nearer to sea level.
How does change in altitude affect your body?
Altitude can also increase your metabolism while suppressing your appetite, meaning you’ll have to eat more than you feel like to maintain a neutral energy balance. When people are exposed to altitude for several days or weeks, their bodies begin to adjust (called “acclimation”) to the low-oxygen environment.
How does the body adjust to a higher altitude *?
The human body can adapt to high altitude through immediate and long-term acclimatization. At high altitude there is lower air pressure compared to a lower altitude or sea-level altitude. … The partial pressure gradients for gas exchange are also decreased, along with the percentage of oxygen saturation in hemoglobin.
What is PO2?
PO2 (partial pressure of oxygen) reflects the amount of oxygen gas dissolved in the blood. It primarily measures the effectiveness of the lungs in pulling oxygen into the blood stream from the atmosphere. Elevated pO2 levels are associated with: Increased oxygen levels in the inhaled air.
How does altitude affect pH?
Blood pH was found to be increased, whereas Po2 and PCo2 levels decreased appreciably under high altitude stress. However, no significant change was observed in plasma bicarbonate level.
What stimulates hyperventilation at altitude?
Hypoxic stimulation of the peripheral chemoreceptors is the chief mechanism for the hyperventilation but there is also evidence that central sensitization of the respiratory centres occurs. Permanent residents of high altitude have a blunted hypoxic ventilatory response compared to acclimatized lowlanders.
What happens to pO2 during hypoventilation?
For example, a decrease in either PO2 of the atmospheric air (changes with altitude) or in alveolar ventilation (hypoventilation) will decrease the amount of fresh air entering the alveoli per unit time. Likewise, an increase in the rate of total body O2 consumption will decrease PO2 in the alveoli.
Does hyperventilation increase oxygen levels?
Our data indicate that venous blood oxygenation level is higher during voluntary breath-holding and lower during hyperventilation.
What happens to the partial pressure of carbon dioxide in the blood during rapid breathing?
During hyperventilation the rate of removal of carbon dioxide from the blood is increased. As the partial pressure of carbon dioxide in the blood decreases, respiratory alkalosis, characterized by decreased acidity or increased alkalinity of the blood, ensues.
How does increased PO2 affect o2 binding to hemoglobin quizlet?
as the partial pressure of carbon dioxide increases, the percent hemoglobin saturation decreases. … PO2 is high, PCO2 is low, pH is high, and temperature is low. All of these factors increase oxygen’s affinity for hemoglobin and therefore oxygen loading occurs and hemoglobin saturation increases.
What is the difference between PO2 and PaO2?
PO2 is just partial pressure of oxgen in a given environment, such as room air. … PAO2 is partial pressure of oxygen in alveoli. PaO2 is partial pressure of oxygen dissolved in (arterial) blood.
What causes right shift in oxyhemoglobin dissociation curve?
Factors which result in shifting of the oxygen-dissociation curve to the right include increased concentration of pCO2, acidosis, raised temperature and high concentrations of 2,3 diphosphoglycerate (2,3 DPG). These factors, in effect, cause the Hb to give up oxygen more readily.
Does hemoglobin affect PaO2?
normal amount of shunting, anemia and hemoglobin variables do not affect PaO2.)
What is the relationship between hemoglobin and Po2 quizlet?
-each heme can bind to 1 o2, so one hemoglobin molecule can carry up to 4 o2. every molecule of it carries 4 o2. relationship between hemoglobin saturation and Po2 shown by this. -as it passes through the alveolar capillaries where the Po2 is high, hemoglobin becomes saturated with oxygen.
What determines partial pressure of oxygen in blood?
The amount of dissolved oxygen within the tissues and the cells depends on several factors including: barometric pressure (BP), climatological conditions (temperature, relative humidity, latitude, altitude), as well as physiological, pathological, and physical-chemical processes within the organism itself [4,5].
What produces the most CO2 on Earth?
- 87 percent of all human-produced carbon dioxide emissions come from the burning of fossil fuels like coal, natural gas and oil. …
- The largest human source of carbon dioxide emissions is from the combustion of fossil fuels.