How often should you switch chest compressors to avoid fatigue
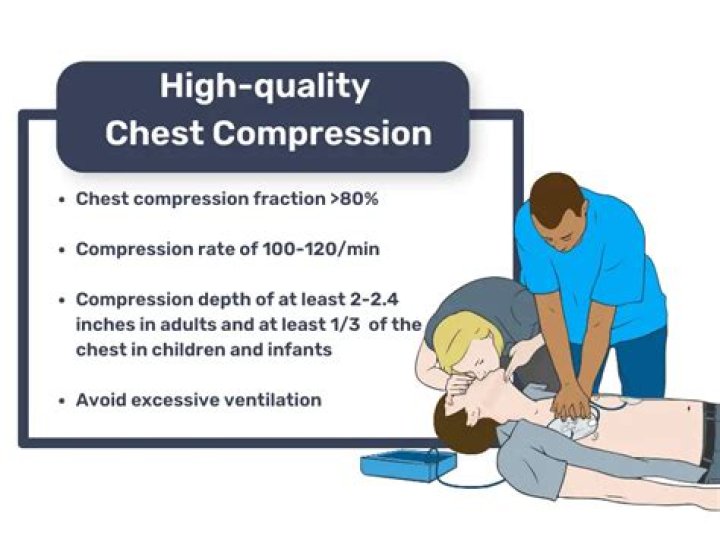
To combat fatigue, CPR guidelines recommend changing the person performing chest compressions every two minutes. However, the process of switching compressors introduces interruptions that have been shown to substantially increase the hands-off time (no-flow ratio), so this is better avoided if possible.
How often should you switch chest compressors to avoid fatigue ACLS?
CPR Quality Change compressor every 2 minutes, or sooner if fatigued. If no advanced airway, 30:2 compression-ventilation ratio.
How often should you switch chest compressors ACLS?
When 2 or more rescuers are available, it is reasonable to switch chest compressors approximately every 2 min (or after about 5 cycles of compressions and ventilation at a ratio of 30:2) to prevent decreases in the quality of compressions. 4.
How often should compressors switch off to prevent fatigue?
The 2 rescuers should change compressor and ventilator roles approximately every 2 minutes to prevent compressor fatigue and deterioration in quality and rate of chest compressions. When multiple rescuers are present, they should rotate the compressor role about every 2 minutes.How often do you switch compressors?
Switch roles after every five cycles of compressions and breaths. One cycle consists of 30 compressions and two breaths for adults. Be sure that between each compression you completely stop pressing on the chest and allow the chest wall to return to its natural position.
What should the 2 rescuers do to keep from getting tired?
Leaning or resting on the chest between compressions can keep the heart from refilling in between each compression and make CPR less effective. Rescuers who become tired may tend to lean on the chest more during compressions; switching roles helps rescuers perform high-quality compressions.
How often should you change compressors in CPR?
The rescuers should change positions every 5th cycle or approximately 2 minutes. Interrupting chest compressions interrupts circulation. During CPR blood flow is provided by chest compressions.
What should you do to prevent getting fatigue while performing CPR?
To combat fatigue, CPR guidelines recommend changing the person performing chest compressions every two minutes. However, the process of switching compressors introduces interruptions that have been shown to substantially increase the hands-off time (no-flow ratio), so this is better avoided if possible.What is the maximum interval for pausing chest compression?
Objectives: Most guidelines recommend pausing chest compressions at 2 min intervals to analyze the cardiac rhythm.
How often should you change rescuers when delivering chest compressions?A: When there is not an AED available the 2 rescuers should switch places every 5 cycles of CPR ( 1 cycle is 30 compressions followed by 2 ventilations ) or every 2 minutes. If an AED has been applied to the unresponsive victim the 2 rescuers will switch every time the AED reanalyzes the cardiac rhythm.
Article first time published onWhat is recommended to minimize interruptions?
To minimize interruptions in chest compressions during CPR, continue CPR while the defibrillator is charging. Immediately after the shock, resume CPR, beginning with chest compressions. Give 2 minutes (about 5 cycles) of CPR.
How often do you bag mask ventilation?
The ventilation should last approximately one second and be provided every five seconds for a target rate of 10 ventilations per minute. Both rescuers should watch the chest for adequate rise, and a third rescuer should periodically auscultate the lungs to ensure adequate ventilation.
How often do you ventilate?
Care should be taken to not over-ventilate the patient. According to the 2015 AHA guidelines update for CPR and ECG, for patients with a perfusing rhythm, ventilations should be delivered once every 5 to 6 seconds (AHA).
How often are rescue breaths given?
Aim to give a rescue breath every 5 to 6 seconds. This is about 10 to 12 breaths per minute. Check to see if the person’s chest rises as you give the first rescue breath. If it doesn’t, repeat step 2 (open the airway) before giving additional rescue breaths.
What is the recommended compression rate?
CPR with rescue breaths Place the heel of your hand on the centre of the person’s chest, then place the other hand on top and press down by 5 to 6cm (2 to 2.5 inches) at a steady rate of 100 to 120 compressions a minute.
How long should it take to switch positions during CPR?
In the two-person resuscitation, rescuers switch positions after about every two minutes. One of the rescuers is positioned near the chest area while the other one is positioned near the head of the victim.
What is BLS prioritize?
Explanation: The 2010 AHA Guidelines for CPR and ECC recommend a change in the BLS sequence of steps from A-B-C (Airway, Breathing, Chest compressions) to C-A-B (Chest compressions, Airway, Breathing) for adults, children, and infants (excluding the newly born; see Neonatal Resuscitation section).
How long should rescue breaths be?
Give 2 gentle puffs or breaths of air instead of a deep breath. Each puff is given 2 seconds apart because each gentle breath should last 1 second. If the chest rises, breathe a gentle puff or breathe into the victim’s mouth a second time. If the chest doesn’t rise, tilt the victim’s head back and chin down again.
When should chest compression be stopped?
A general approach is to stop CPR after 20 minutes if there is no ROSC or viable cardiac rhythm re-established, and no reversible factors present that would potentially alter outcome.
When do you pause in compression?
Summary: It is important to avoid any unnecessary pause in chest compressions before and after a defibrillation shock. Pauses should be kept to an absolute minimum, preferably to less than 10 s.
How do you ventilate a patient with Perfusing rhythm?
For ventilation of patients with a perfusing rhythm (ie, better pulmonary blood flow than is present during CPR), deliver approximately 10 to 12 breaths per minute (1 breath every 6 to 7 seconds). Deliver these breaths over 1 second when using a mask or an advanced airway.
What effect can rescuer fatigue have on chest compressions?
The fatigue of the rescuer during CPR affects the quality of the chest compressions. After the start of continuous chest compressions, the depth of chest compressions decreases over time due to the fatigue of the rescuer.
What is Drsabcd?
DRSABCD is an acronym/mnemonic taught on first aid courses to help you have an action plan on how to respond in a medical emergency. It >stands for Danger, Response, Send for help, Airway, Breathing, Cardiopulmonary resuscitation (CPR) and Defibrillation.
How often is CPR effective outside of a hospital?
Recent statistics have shown that the earlier CPR is performed, the higher the chances of survival after cardiac arrest. Nearly 45 percent of out-of-hospital cardiac arrest victims survived when bystander CPR was administered.
Why should you minimize interruptions in chest compressions?
Fewer interruptions in chest compression–supported circulation during cardiac arrest result in more perfusion to the heart and central nervous system, which culminates in better outcome.
What is chest compression feedback monitor?
A: An instrumented directive feedback device measures compression rate, depth, hand position, recoil, and chest compression fraction and provides real-time audio or visual feedback (or both) on these critical CPR skills.
What do you do after AED shock?
Begin CPR after delivering the shock. If no shock is advised, begin CPR right away. Perform 2 minutes (about 5 cycles) of CPR and continue to follow the AEDs prompts. If you notice obvious signs of life, discontinue CPR and monitor breathing for any changes in condition.
How long do you squeeze the bag to ventilate?
Squeeze the entire bag over 1-2 seconds and then release the bag. Each ventilation must be a minimum of 800cc. Assure appropriate chest rise during ventilations. Continue to ventilate the patient for 30 seconds prior to attaching the oxygen.
What is the most effective way to deliver bag mask ventilation?
“Bag-mask ventilation is most effective when provided by 2 trained and experienced rescuers. One rescuer opens the airway and seals the mask to the face while the other squeezes the bag. Both rescuers watch for visible chest rise.”
How do I improve my bag mask ventilation?
To mask ventilate, obtain a good seal with the mask with one hand and then squeeze the bag with the other. The chest should rise with each breath. Pay attention to the resistance you feel as the lungs inflate. Obstruction makes squeezing the bag difficult.
How many times per minute should a child be ventilated?
The rescuer delivering the rescue breaths (ventilations) should give 8 to 10 breaths per minute for infants and should be careful to avoid delivering an excessive number of ventilations. A ventilation rate of about 8 to 10 breaths per minute will be the equivalent of giving 1 breath about every 6 to 8 seconds.



