How often should you ventilate an apneic patient
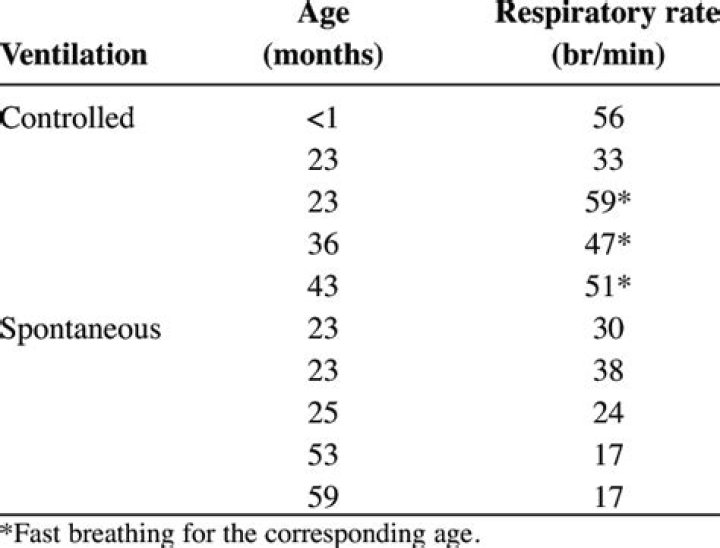
After supplemental oxygen has been attached, the candidate must ventilate the patient at a rate of 10 – 12 ventilations/minute (1 ventilation every 5 – 6 seconds) with adequate volumes of oxygen-enriched air.
How often should you ventilate a patient with a BVM?
Ventilate the patient. The ventilation should last approximately one second and be provided every five seconds for a target rate of 10 ventilations per minute. Both rescuers should watch the chest for adequate rise, and a third rescuer should periodically auscultate the lungs to ensure adequate ventilation.
How often should adults be ventilated?
Ventilate the patient at a rate of 10-12 times per minute (every 5-6 seconds).
When ventilating an apneic patient with a bag mask device each breath should be delivered over?
Rationale: When ventilating any apneic patient with a bag-valve mask, you should squeeze the bag over a period of 1 second and observe for visible chest rise. Ventilate the apneic adult at a rate of 10 to 12 breaths/min (one breath every 5 seconds).When do you use CPAP EMT?
It should be used on patients who are alert and able to follow commands, show signs of respiratory distress, have rapid breathing, and a pulse oximetry of less than 90%.
How long should you suction a patient Nremt?
Do not suction too long! The maximum suction time should only be 15 seconds. After suctioning, re-oxygenate the patient.
What is apneic patient?
: of, relating to, or affected by apnea : involving or exhibiting transient cessation of respiration Obstructive sleep apnea is the intermittent interruption of airflow through the nose and mouth that occurs during sleep and is considered present when individuals have more than 5 apneic episodes per hour of sleep.—
How often do you ventilate a patient with a perfusing rhythm?
According to the 2015 AHA guidelines update for CPR and ECG, for patients with a perfusing rhythm, ventilations should be delivered once every 5 to 6 seconds (AHA).How do Emts passive ventilation?
In the passive ventilation approach, EMS providers generally deliver three cycles of 200 continuous chest compressions with a rhythm analysis and defibrillation attempt after every two hundred compressions and ventilation occurs passively through elastic recoil of the patient’s chest [56-60].
How many times per minute should a child be ventilated?The rescuer delivering the rescue breaths (ventilations) should give 8 to 10 breaths per minute for infants and should be careful to avoid delivering an excessive number of ventilations. A ventilation rate of about 8 to 10 breaths per minute will be the equivalent of giving 1 breath about every 6 to 8 seconds.
Article first time published onWhat is the preferred method of ventilating a patient?
In order of preference, the methods for ventilating a patient by the EMT- Basic are as follows: 1. Mouth-to-mask with supplemental oxygen 2. Two person bag-valve-mask 3. Flow restricted, oxygen powered ventilation device 4.
How does CPAP improve oxygenation and ventilation in patients with certain respiratory problems?
In CPAP no additional pressure above the set level is provided, and patients are required to initiate all of their breaths. The application of CPAP maintains PEEP, can decrease atelectasis, increases the surface area of the alveolus, improves V/Q matching, and hence, improves oxygenation.
In which of the following situations should you perform the jaw thrust maneuver?
The jaw-thrust maneuver is often used on patients with cervical neck problems or suspected cervical spine injury. The maneuver is used on a supine patient.
What are signs of inadequate breathing?
- Breathing rate. An increase in the number of breaths per minute may mean that a person is having trouble breathing or not getting enough oxygen.
- Color changes. …
- Grunting. …
- Nose flaring. …
- Retractions. …
- Sweating. …
- Wheezing. …
- Body position.
What is the correct ventilation rate?
It is critically important that rescuers maintain a ventilation rate of 8 to 10 breaths per minute during CPR and avoid excessive ventilation.
What does it mean when ETCO2 is low?
Low ETCO2 with other signs of shock indicates poor systemic perfusion, which can be caused by hypovolemia, sepsis or dysrhythmias. Cardiac arrest is the ultimate shock state; there is no circulation or metabolism and no CO2 production unless effective chest compressions are performed.
When delivering rescue breaths to any non breathing patient you should?
To give rescue breaths, tilt their head back and seal your mouth over either their mouth or nose. Blow air into them with two steady breaths. If you are breathing into the mouth, pinch the nose.
Can you use a CPAP as a ventilator in an emergency?
Can I use a CPAP machine as a ventilator? CPAP devices are designed to provide only PAP (positive airway pressure) and would require significant rework in order to function as a ventilator.
How long are Covid patients on CPAP?
Median (IQR) CPAP duration was 4 (1–8) days, while hospital length of stay was 16 (9–27) days. 60-day in-hospital mortality was 34% (95% CI 0.304–0.384%) overall, and 21% (95% CI 0.169–0.249%) and 73% (95% CI 0.648–0.787%) for full treatment and DNI subgroups, respectively.
How many LPM is EMS CPAP?
BACKGROUND: CPAP is frequently used in prehospital and emergency settings. An air-flow output minimum of 60 L/min and a constant positive pressure are 2 important features for a successful CPAP device.
What is apneic oxygenation?
Apnoeic oxygenation involves the mass flow of a high fraction of inspired oxygen, aided by flushing of dead space, generation of positive airway pressure and cardiogenic oscillations. Higher flow rates can enable clearance of carbon dioxide.
Does apnea mean not breathing?
Apnea is the medical term used to describe slowed or stopped breathing. Apnea can affect people of all ages, and the cause depends on the type of apnea you have. Apnea usually occurs while you’re sleeping.
How often can you suction a patient?
There is no clear consensus on how frequently an individual should be suctioned. It is patient dependent on the amount of secretions and their ability to clear the secretions independently. Airway patency can be checked by attempting suctioning at least every 8 hours.
How often do you suction endotracheal tube?
Frequency of Suctioning It has been suggested by Pedersen et al3 that ETS should be performed at least every 8 hours to slow the formation of the secretion biofilm within the lumen of the endotracheal tube (ETT).
How long should an EMT suction for?
While suctioning, use a sweeping motion to retract the suction catheter. Limit suctioning to no longer than 15 seconds.
When is positive pressure ventilation used?
NIPPV can be used in acute hypercapnic respiratory failure so long as the patient’s condition is responsive to this form of therapy. Conditions that respond the most to NIPPV include exacerbations of chronic obstructive pulmonary disease (COPD) and acute cardiogenic pulmonary edema.
How does passive ventilation work?
How passive ventilation works. Passive ventilation uses doors, windows, vents, louvres and other openings to bring fresh air into your home and let stale air out. … In winter, well-designed passive ventilation refreshes the air in your home without creating draughts or letting out too much heat.
What is active ventilation EMT?
Ventilation is the process of air moving in and out of the lungs. Oxygenation refers to the diffusion of oxygen from the alveolus into the blood. Ventilation is an active process, meaning the lungs cannot ventilate without the actions of the respiratory muscles (or mechanical ventilator with the intubated patient).
How often should you deliver breaths during CPR with an endotracheal tube in place?
When an advanced airway (eg, endotracheal tube, esophageal-tracheal combitube [Combitube], or laryngeal mask airway [LMA]) replaces the face mask, rescuers should deliver 8 to 10 breaths per minute during CPR.
When ventilating patients without an advanced airway should you always?
In the absence of an advanced airway during CPR, current guidelines based on very limited evidence recommend two positive pressure breaths after every 30 chest compressions. These breaths should be of an inspiratory time of 1 s and produce a visible chest wall rise [59].
Why is airway maintenance so important during CPR?
The priorities of airway management during cardiopulmonary resuscitation are to minimise interruptions in chest compressions, to optimise blood flow and oxygen delivery to vital organs and to minimise delays in defibrillation if the initial rhythm is shockable.