How would you describe gingiva
The tissue of the upper and lower jaws that surrounds the base of the teeth. Also called gums. Anatomy of the oral cavity.
How would you describe an inflamed gingiva?
Gingivitis can cause dusky red, swollen, tender gums that bleed easily, especially when you brush your teeth. Healthy gums are firm and pale pink and fitted tightly around the teeth.
What is the normal color of gingiva?
What color is the human gingiva? It is frequently described as “coral pink” and is dependent upon the thickness of epithelium, the degree of keratinization, the magnitude of pigmentation, and the underlying vascularization1.
What is the function of the gingiva?
Gingival Structure, Function, and the Latest Research The gingiva (or gums) is the tissue that surrounds and protects the teeth and underlying bone. The gingiva is attached to the tooth, forming a seal that protects the underlying bone and helps provide a barrier against infection.What is gingiva in anatomy?
gum, also called gingiva, plural gingivae, in anatomy, connective tissue covered with mucous membrane, attached to and surrounding the necks of the teeth and adjacent alveolar bone. Before the erupting teeth enter the mouth cavity, gum pads develop; these are slight elevations of the overlying oral mucous membrane.
What is erythematous gingiva?
A condition in which the edge of the gums near the teeth become red and inflamed. Linear gingival erythema is common with HIV infection.
How do you find gingival consistency?
The consistency of marginal and interdental gingiva should be firm when palpated with the side of a blunt instrument, such as a periodontal probe. In the presence of inflammation, the gingiva may be soft and spongy, swollen, shiny, and easily deflected away from the tooth with an instrument or a blast of air.
What Innervates the gingiva?
The innervation of the oral gingiva is unique because all the nerves supplying the gingival mucosa originate from the mandibular and maxillary branches of the trigeminal nerve (CN V).What are the cells of gingiva?
4 Gingival Stem Cells. The gingival tissue is composed of both epithelial and mesenchymal cells, and MSC-like cells have been cultured from gingival tissue (Fournier et al., 2010; Hsu, Huang, & Feng, 2012; Mitrano et al., 2010; Widera et al., 2009).
What is gingiva made of?The gingiva is composed of fibrous tissue covered by mucous membrane that is firmly attached to the periosteum of the alveolar processes of the mandible and maxilla. The lower gingiva includes the mucosa covering the mandible from the gingival-buccal gutter to the origins of the mobile mucosa on the floor of the mouth.
Article first time published onHow do you describe gingival appearance?
Healthy gingiva is described as ‘salmon’ or ‘coral pink’. It may be pigmented, which reflects the ethnic origin of the subject. The gingiva is firm in consistency and firmly attached to the underlying alveolar bone. The surface of gingiva is keratinised and may exhibit an orange peel appearance, called ‘stippling’.
Why gingiva is scalloped?
Thin gingival tissue is associated with a thin band of the keratinized tissue, scalloped gingival contour suggestive of thin bony architecture and is more sensitive to inflammation and trauma.
Why is gingiva light pink?
Anemia occurs when you don’t have enough healthy red blood cells in your body. Red blood cells are responsible for carrying oxygen to your body’s organs and tissues. When your gum tissue doesn’t get enough oxygen, it may turn pale.
What is the alveolar process?
The alveolar process is the horizontal portion of the maxilla that holds the tooth roots. b. Alveoli for the tooth roots are present all along the alveolar process, except where these have been resorbed following the loss of teeth.
Which term describes the space between the tooth and the free gingiva?
The gingival sulcus is an area of potential space between a tooth and the surrounding gingival tissue and is lined by sulcular epithelium. The depth of the sulcus (Latin for groove) is bounded by two entities: apically by the gingival fibers of the connective tissue attachment and coronally by the free gingival margin.
What is the alveolar ridge?
The alveolar ridge is a small protuberance just behind the upper front teeth that can easily be felt with the tongue. The major part of the roof of the mouth is formed by the hard palate in the front, and the soft palate or velum at…
Why gingiva is firm and resilient?
39. Consistency: The gingiva is firm & resilient with exception of the movable free margin, tightly bound to underlying bone. The collagenous nature of lamina propria & its contiguity with mucoperiosteum of alveolar bone determines the firmness of attached gingiva. Resilient is due to gingival fibers.
What is shape of gingiva?
In health, the marginal gingiva follows the scalloped pattern established by the contour of the cementoenamel junction (CEJ) of the teeth. 2. The part of the gingival tissue that fills in the triangular-shaped spaces between the teeth is the interdental papilla.
Why normal gingiva is not identical with clinically healthy gingiva?
The gingival sulcus, or crevice, is therefore created between tooth and mucosa; its depth varies from 0.1 to 0.3 cm. The attached gingiva extends from the free gingival groove to the beginning of the alveolar crest and is continuous with the alveolar mucosa.
What is edematous gingiva?
Enlargement of marginal and interproximal gingival tissues. Results from collagen loss and an accumulation of interstitial fluid. Tissues are easily compressed with a blunt instrument. Diffuse redness.
Why is erythematous gingiva red?
Linear gingival erythema is a condition that’s related to a fungal infection of the gums. It appears as a red line along the gum line and causes pain and sometimes bleeding. This condition is one of the most common oral complications of HIV.
What is gingival ulceration?
Gingival ulceration is the result of irritating materials that contact the peridental tissues for extended periods of time.
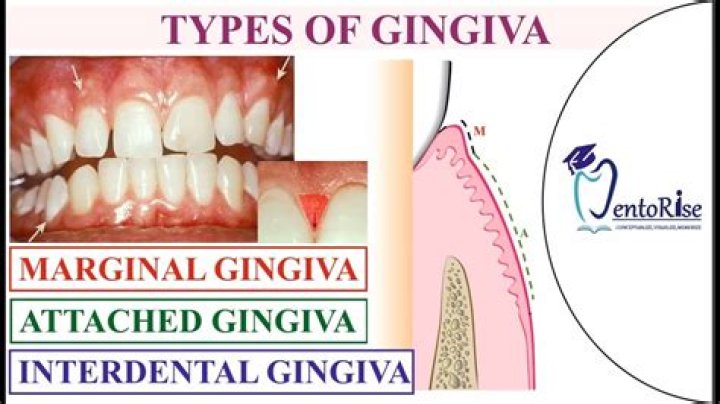
What are the types of gingiva?
There are two types of gingivae that are clearly recognizable and they are known as the marginal gingiva that is mobile, and the attached gingiva.
What is the junction of the lips and the gingiva called?
A mucogingival junction is an anatomical feature found on the intraoral mucosa. The mucosa of the cheeks and floor of the mouth are freely moveable and fragile, whereas the mucosa around the teeth and on the palate are firm and keratinized.
Which gingiva is Keratinized?
Attached gingiva – This tissue is adjacent to the free gingiva and is keratinized and firmly attached to the bone structure. It can range from 3-12 mm in height. Free gingiva – This tissue is not attached and forms a collar around the tooth.
Is gingiva hard or soft tissue?
Structure. The gums are part of the soft tissue lining inside the mouth. The gums surround the base of the teeth and act as a seal. Unlike the soft tissues lining found on the lips and cheeks, most of the gums are tightly bound to the underlying bone.
What is the blood supply to the gingiva?
Consequently, the submental artery can be considered the main arterial blood supply to the floor of the mouth and mandibular lingual gingiva.
What is alveolar artery?
The inferior alveolar artery is a branch of the maxillary artery. It runs with the inferior alveolar nerve as it descends through the infratemporal fossa and enters the mandibular canal and supplies mandibular teeth. In the region of the first premolar it bifurcates into the incisive and mental branches.
What is alveolar gingiva?
alveolar gingiva attached gingiva. areolar gingiva the portion attached to the alveolar process by loose areolar connective tissue. attached gingiva that portion of the gingiva which is firm and resilient and is bound to the underlying cementum and the alveolar bone, thus being immovable. Called also alveolar gingiva.
What is rolled gingiva?
Rolled – thickening of the gingival margin with inflammatory edema at the necks of the teeth. G. Bulbous – fills gingival embrasure but is no longer pyramidal shaped; swollen, rounded rather than sharp peak; covers part of facial or lingual surface of tooth.
What is gingival phenotype?
Periodontal phenotype is determined by gingival phenotype defined as three-dimensional volume of the gingiva and by bone morphotype (thickness of the buccal bone plate) [11]. There is evidence reporting a correlation between gingival thickness and buccal bone plate [12].