Is impetigo Gram positive or negative
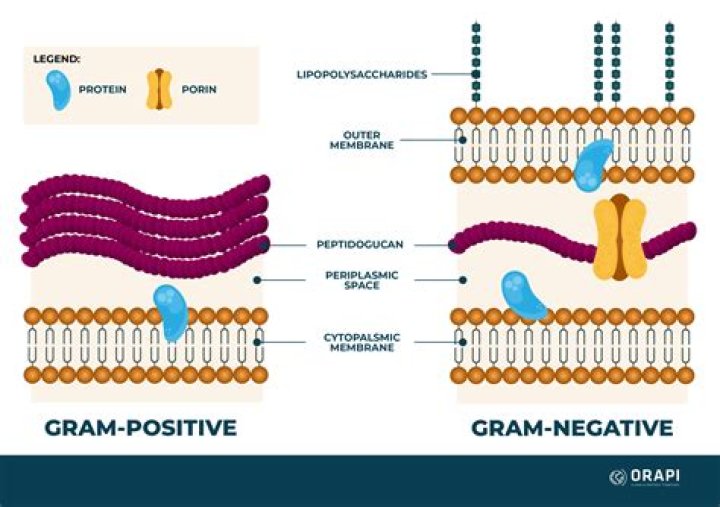
pyogenes, or both cause non-bullous impetigo, which is also called “impetigo contagiosa.” S. pyogenes are gram-positive cocci that grow in chains (see Figure 1). They exhibit β-hemolysis (complete hemolysis) when grown on blood agar plates.
Is impetigo a virus or bacteria?
What is impetigo? Impetigo is a common bacterial skin infection caused by Group A Streptococcus (GAS) or “strep.”
Is group A streptococcus Gram positive or negative?
Streptococci are a large group of gram-positive, nonmotile, non–spore-forming cocci about 0.5-1.2µm in size. They often grow in pairs or chains and are negative for oxidase and catalase. S pyogenes tends to colonize the upper respiratory tract and is highly virulent as it overcomes the host defense system.
What type of pathogen is impetigo?
Impetigo is a skin infection caused by one or both of the following bacteria: group A Streptococcus and Staphylococcus aureus.What cells does impetigo affect?
Impetigo involves the epidermis and is seen mostly in preschool children. It is caused by two microorganisms: S. aureus and GAS. Other bacterial infections that involve deeper parts of the skin are erysipelas and cellulitis.
Can you get impetigo twice?
Anyone can get impetigo — and more than once, Smith says. Although impetigo is a year-round disease, it occurs most often during the warm weather months.
How is impetigo diagnosed?
To diagnose impetigo, your doctor might look for sores on your face or body. Lab tests generally aren’t needed. If the sores don’t clear, even with antibiotic treatment, your doctor might take a sample of the liquid produced by a sore and test it to see what types of antibiotics would work best on it.
Can impetigo be systemic?
5 Bullous impetigo favors moist, intertriginous areas, such as the diaper area, axillae, and neck folds. Systemic symptoms are not common but may include weakness, fever, and diarrhea. Most cases are self-limited and resolve without scarring in several weeks.Is impetigo aerobic or anaerobic?
Skin microflora consists mainly of aerobic diphtheroids (Corynebacterium spp.), anaerobic diphtheroids (Propionibacterium acnes) and coagulase negative staphylococci (Staphylococcus epidermidis). Recent genetic studies have shown a large quantity of Pseudomonas spp. and Janthinobacterium spp.
Is impetigo a secondary infection?Impetigo may be classed as primary or secondary: In primary impetigo, the infection affects healthy skin. In secondary impetigo, the infection affects skin that is already ‘broken’ by another skin condition. For example, skin with eczema, psoriasis or a cut sometimes develops a secondary impetigo.
Article first time published onIs Staph aureus Gram positive?
Staphylococcus aureus is a gram-positive bacteria that cause a wide variety of clinical diseases. Infections caused by this pathogen are common both in community-acquired and hospital-acquired settings.
Can gram positive microorganisms appear gram-negative?
If the decolorizing agent is applied on the cell for too long time, the Gram-positive organisms to appear Gram-negative. Under-decolorization occurs when the alcohol is not left on long enough to wash out the CV-I complex from the Gram-negative cells, resulting in Gram-negative bacteria to appear Gram-positive.
Is Strep pyogenes Gram positive?
Streptococci are gram-positive, catalase-negative, coagulase-negative cocci that occur in pairs or chains. They are divided into three groups by the type of hemolysis on blood agar: beta-hemolytic (complete lysis of red cells), a hemolytic (green hemolysis), and gamma-hemolytic (no hemolysis).
Is cellulitis caused by Gram positive or negative?
Gram-negative bacillary (rod) cellulitis, like P. aeruginosa, is common among hospitalized, immunocompromised patients and may have multidrug resistance.
What type of lesions is impetigo?
6 Impetigo starts as maculopapular lesions that transition into thin-walled vesicles that rapidly rupture, leaving superficial, sometimes pruritic or painful erosions covered by the classic honey-colored crusts4,8 (Figure 1). The course of infection can last two to three weeks if untreated.
What blood test indicates bacterial infection?
A procalcitonin test measures the level of procalcitonin in your blood. A high level could be a sign of a serious bacterial infection, such as sepsis. Sepsis is the body’s severe response to infection.
What is the most common cause of impetigo?
It’s usually caused by one of two bacteria: Staphylococcus aureus or Streptococcus pyogenes (also called group A streptococcus, which also causes strep throat). Methicillin-resistant Staphylococcus aureus (MRSA) is also becoming an important cause of impetigo.
What is the difference between impetigo and tinea?
Tinea is a very common and often missed mimic. Careful and full skin examination is required to rule out tinea as a cause of impetigo-like infection of the skin. Unlike impetigo, tinea almost never occurs on the upper lip. Herpetic impetigo also is a very common and often missed mimic.
Is impetigo lifelong?
The most common is Staphylococcus aureus, also called staph. Streptococci bacteria can also cause impetigo. Many people have these kinds of bacteria on their body from time to time. A smaller number of people have lifelong (permanent) colonies of these harmful bacteria on their skin.
How do you know if impetigo is healing?
- It usually starts with reddish, itchy sores around the mouth and nose.
- The sores break open, leaving red and irritated skin around them.
- A brownish-yellow crust forms.
- When the crusts heal, there are reddish spots that fade and don’t leave scars.
How serious is impetigo?
Impetigo isn’t usually serious and often clears up without treatment after two to three weeks. Treatment is often recommended as it can help clear up the infection in around seven to 10 days and reduce the risk of the infection being passed on to others.
Does coconut oil help impetigo?
“It’s usually a small, localized infection in a small area, and it’s very easily treated with a topical antibiotic,” Oza says. There are some reports that home-based remedies, such as tea tree oil, coconut oil, and Manuka honey, also work to treat impetigo.
Is gangrene aerobic or anaerobic?
Gas gangrene is caused by an anaerobic, gram-positive, spore-forming bacillus of the genus Clostridium. C perfringens is the most common etiologic agent that causes gas gangrene.
What skin lesions are characteristic for impetigo bullosa?
Fragile, clear or cloudy bullae (Fig. 10.1A) are characteristic of bullous impetigo. A thin, varnish-like crust occurs after rupture of the bulla. A delicate, collarette-like remnant of the blister roof is often present at the rim of the crust.
How does impetigo affect the integumentary system?
Key points about impetigo in children Impetigo is an infection that affects the skin. It’s caused by bacteria. It causes skin sores. The sores may be red and painful, and contain fluid called pus.
Does azithromycin treat impetigo?
If someone has a penicillin allergy, the treatment is usually with erythromycin (or other similar medicines such as clarithromycin [Biaxin] or azithromycin [Zithromax]). For some infections caused by resistant bacteria, clindamycin or trimethoprim-sulfamethoxazole (Bactrim) may be required.
What is extensive impetigo?
Impetigo causes blister-like sores. The sores can fill with pus and form scabs, and scratching can spread the infection. Impetigo is caused by bacteria. It is contagious and usually occurs in children. It is the most common bacterial skin infection presented by children to primary care physicians.
What is the drug of choice for impetigo?
Systemic Antibiotic Treatment Beta-lactamase‒resistant antibiotics (eg, cephalosporins, amoxicillin-clavulanate, dicloxacillin) are recommended as S aureus isolates from impetigo are usually methicillin-susceptible. Cephalexin appears to be the drug of choice for oral antimicrobial therapy in children.
What is impetigo NZ?
Impetigo (you say, im-pa-ty-go), also known as school sores, is a common skin infection caused by bacteria. The infection causes blisters on exposed parts of body, such as hands and face, especially around the nose and mouth. The blisters burst and turn into a sore with a yellow crust.
Is Staph aureus coagulase positive or negative?
Classification. S aureus and S intermedius are coagulase positive. All other staphylococci are coagulase negative. They are salt tolerant and often hemolytic.
Is Staphylococcus Saprophyticus Gram positive or negative?
Staphylococcus saprophyticus is a Gram-positive, coagulase-negative, non-hemolytic coccus that is a common cause of uncomplicated urinary tract infections (UTIs), particularly in young sexually active females.