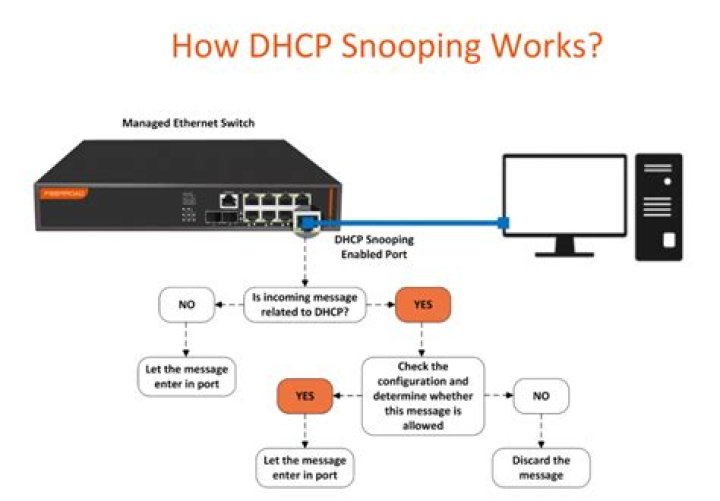
What does incentive spirometry mean
Your health care provider may recommend that you use an incentive spirometer after surgery or when you have a lung illness, such as pneumonia. The spirometer is a device used to help you keep your lungs healthy. Using the incentive spirometer teaches you how to take slow deep breaths.
What is incentive spirometer used for?
Your health care provider may recommend that you use an incentive spirometer after surgery or when you have a lung illness, such as pneumonia. The spirometer is a device used to help you keep your lungs healthy. Using the incentive spirometer teaches you how to take slow deep breaths.
What is a normal incentive spirometry value?
Normal values in healthy males aged 20-60 range from 4.5 to 3.5 liters, and normal values for females aged 20-60 range from 3.25 to 2.5 liters.
What does incentive spirometry mean in medical terms?
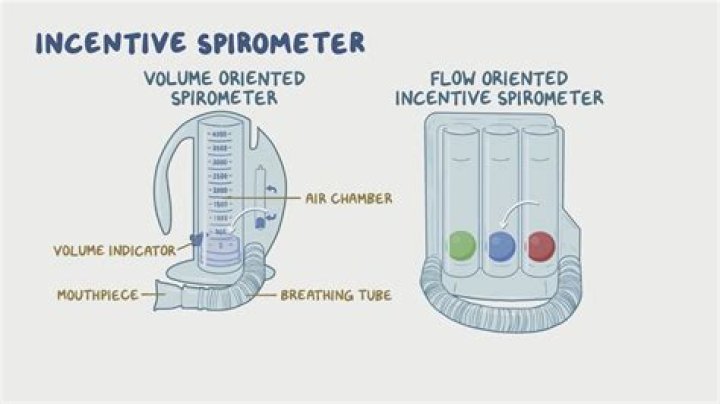
An incentive spirometer is a handheld medical device that measures the volume of your breath. It helps your lungs recover after surgery or lung illness, keeping them active and free of fluid. A piston rises inside the device to measure your breath volume when you breathe from an incentive spirometer.What are the two types of incentive spirometry?
Two types of incentive spirometry are commercially available: volume-oriented incentive spirometry (VIS) and flow-oriented incentive spirometry (FIS). Both VIS and FIS are used to encourage the patient to inhale to lung capacity through maximal inspiration aided with visual feedback.
How is spirometry different from asthma and COPD?
Also, like asthmatics, patients with COPD will have a reduction in their ability to exhale, and will show reductions in airflow when tested with spirometry. However, unlike asthmatic patients, COPD patients will not be able to completely correct their lung function even with treatment.
Is incentive spirometry effective?
We conclude that incentive spirometry is a relatively good measure of lung function and may be used to assess respiratory recovery in the days after thoracic surgery.
Is atelectasis serious?
Large areas of atelectasis may be life threatening, often in a baby or small child, or in someone who has another lung disease or illness. The collapsed lung usually reinflates slowly if the airway blockage has been removed. Scarring or damage may remain. The outlook depends on the underlying disease.Does using a spirometer help COPD?
Spirometry can detect COPD even in its earliest stage, even before any obvious symptoms are noticeable. Along with diagnosing COPD, this test can also help track progression of the disease, assist in staging, and even help to determine treatments that might be most effective.
Why is incentive spirometer important after surgery?Using your incentive spirometer after surgery will help you keep your lungs clear. The incentive spirometer will also help keep your lungs active when you are recovering from surgery, as if you were at home performing your daily activities.
Article first time published onWhat is a good score on a spirometry test?
Normal results are 70% or more for adults under 65. FVC/FEV-1 ratios below normal help your doctor rate the severity of your lung condition: Mild lung condition: 60% to 69% Moderate lung condition: 50% to 59%
What is a good spirometry number?
Generally speaking, a healthy FEV1% for adults is above 70%, while a healthy FEV1% for children is 80-85%.
What is a good lung capacity reading?
Lung volume is measured in litres. Your predicted total lung capacity (TLC) is based on your age, height, sex and ethnicity, so results will differ from person to person. Normal results typically range between 80% and 120% of the prediction.
How does incentive spirometry prevent atelectasis?
Incentive spirometry is designed to mimic natural sighing or yawning by encouraging the patient to take long, slow, deep breaths. This decreases pleural pressure, promoting increased lung expansion and better gas exchange. When the procedure is repeated on a regular basis, atelectasis may be prevented or reversed.
What is the normal lung capacity?
Among healthy adults, the average lung capacity is about 6 liters. Age, gender, body composition, and ethnicity are factors affecting the different ranges of lung capacity among individuals.
Which situation will happen when you have emphysema?
In emphysema, the inner walls of the lungs’ air sacs (alveoli) are damaged, causing them to eventually rupture. This creates one larger air space instead of many small ones and reduces the surface area available for gas exchange. Emphysema is a lung condition that causes shortness of breath.
Can spirometry detect asthma?
Spirometry is used to diagnose asthma, chronic obstructive pulmonary disease (COPD) and other conditions that affect breathing. Spirometry may also be used periodically to monitor your lung condition and check whether a treatment for a chronic lung condition is helping you breathe better.
What are the signs of dying from COPD?
- Chest pain due to lung infections or coughing.
- Trouble sleeping, especially when lying flat.
- Foggy thinking because of lack of oxygen.
- Depression and anxiety.
What is the life expectancy of someone with COPD?
Depending on the disease severity, the five-year life expectancy for people with chronic obstructive pulmonary disease (COPD) ranges from 40%-70%. That means 40-70 out of 100 people will be alive after five years of diagnosis of COPD. COPD is a chronic, gradually progressing lung disease that is not completely curable.
Is incentive spirometer good for emphysema?
Conclusion: The use of IS appears to improve arterial blood gases and health-related quality of life in patients with COPD exacerbations, although it does not alter pulmonary function parameters.
How can I test myself for COPD?
It’s simple and painless. You will be asked to take a deep breath, and you’ll blow hard into a mouthpiece that’s connected to a small machine. That machine, called the spirometer, measures how fast you blow air out of your lungs. Results can tell you whether you have COPD, even if you haven’t gotten symptoms yet.
How can I test my lung capacity at home?
- Set the pointer. …
- Attach the mouthpiece to the meter. …
- Sit up or stand up as straight as you can, and take a deep breath.
- Close your lips tightly around the mouthpiece. …
- Breathe out as hard and as fast as you can for 1 or 2 seconds. …
- Write down the number on the gauge. …
- Repeat these steps 2 more times.
What are the 3 types of atelectasis?
There are three major types of atelectasis: adhesive, compressive, and obstructive.
What is the most common cause of atelectasis?
Atelectasis occurs from a blocked airway (obstructive) or pressure from outside the lung (nonobstructive). General anesthesia is a common cause of atelectasis. It changes your regular pattern of breathing and affects the exchange of lung gases, which can cause the air sacs (alveoli) to deflate.
How do you fix atelectasis?
Atelectasis treatment can include breathing or coughing exercises, inhaled medicines, breathing devices, or surgery. Atelectasis usually gets better with time or treatment. However, if it is undiagnosed or untreated, serious complications can occur, including fluid buildup, pneumonia, and respiratory failure.
Does incentive spirometer reduce fever?
By: Linh Tran, RN. An Incendve spirometer is a breathing device that helps expand the lungs and is encouraged after surgery to help prevent pulmonary complicadons , such as pneumonia, atelectasis, and fever.
When do you not use an incentive spirometer?
If you have an active respiratory infection (such as pneumonia, bronchitis, or COVID-19) do not use the device when other people are around.
How long should I use spirometer after surgery?
- At the hospital: You will need to use the incentive spirometer 10 times every hour you are awake after surgery.
- At home: You will need to use the incentive spirometer 10 times every two hours for your first seven days at home.
How is COPD diagnosed with spirometry?
The most effective and common method for diagnosing COPD is spirometry. It’s also known as a pulmonary function test or PFT. This easy, painless test measures lung function and capacity. To perform this test, you’ll exhale as forcefully as possible into a tube connected to the spirometer, a small machine.
What does 70 lung capacity mean?
If the FVC and the FEV1 are within 80% of the reference value, the results are considered normal. The normal value for the FEV1/FVC ratio is 70% (and 65% in persons older than age 65). When compared to the reference value, a lower measured value corresponds to a more severe lung abnormality.
Is COPD a disability for Social Security?
If you or a loved one has COPD, there may be financial resources available. If your COPD causes you to be out of work for at least 12 months, then yes, you could qualify for Social Security Disability Insurance (SSDI).