What is 6 Ps nursing
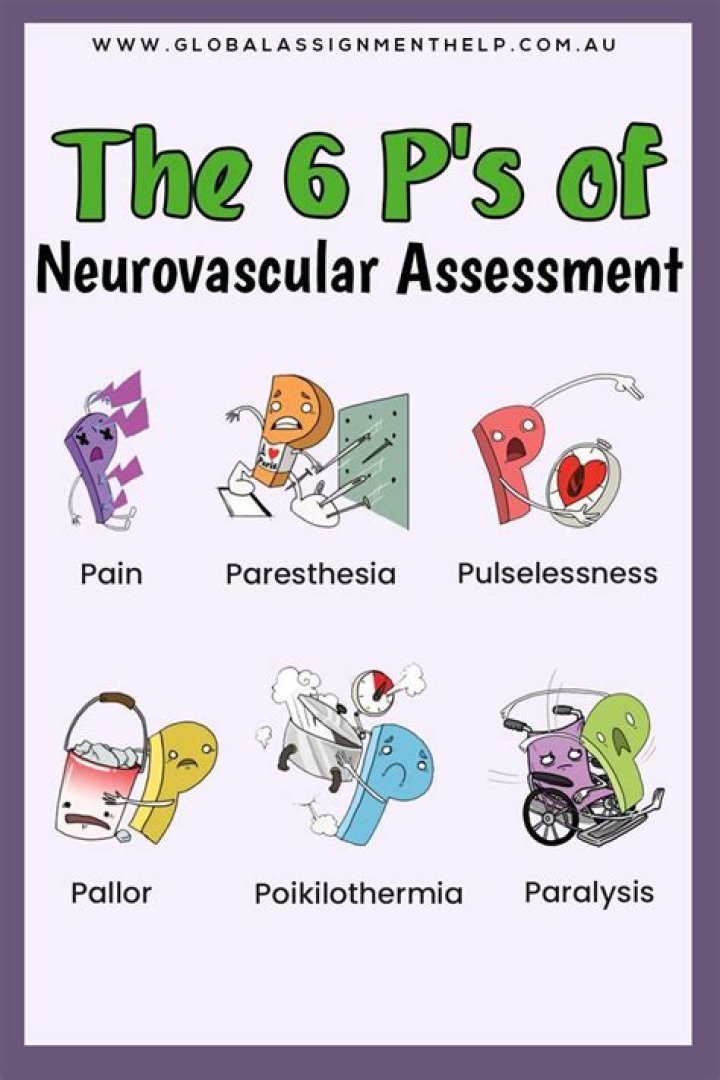
The six P’s include: (1) Pain, (2) Poikilothermia, (3) Paresthesia, (4) Paralysis, (5) Pulselessness, and (6) Pallor. The earliest indicator of developing ACS is severe pain.
What are the 6 P's of patient care?
The six Ps include: Pain, Position, Personal care needs, Proximity of belongings, Pumps and Promise.
What are the 5 P's in nursing care?
When assessing for neurovascular integrity, remember the five Ps: pallor, pain, pulse, paralysis and paraesthesia.
What are the 6 P's of neurovascular assessment and what do they mean?
Terms in this set (6) Pain. due to ischemia. Pallor. due to impaired circulation. Pulselessness.What are the 5 P's of compartment syndrome?
Common Signs and Symptoms: The “5 P’s” are oftentimes associated with compartment syndrome: pain, pallor (pale skin tone), paresthesia (numbness feeling), pulselessness (faint pulse) and paralysis (weakness with movements). Numbness, tingling, or pain may be present in the entire lower leg and foot.
What are the 5 P's of fall prevention?
During hourly rounds with patients, our nursing and support staff ask about the standard 5 Ps: potty, pain, position, possessions and peaceful environment.
What does CI CARE stand for?
It is a communication tool, developed by UCLA Health System and used by Stanford Health. It has been proven to promote positive interactions from beginning to end. CICare stands for: … Communicate what you’re going to do (to understand, clarify and anticipate needs and expectations)
What is pressure compartment syndrome?
Compartment syndrome occurs when increased pressure within a compartment compromises the circulation and function of the tissues within that space [1,2]. Compartment syndrome may occur acutely, often following trauma, or as a chronic syndrome, seen most often in athletes, that presents as insidious pain.Who performs a fasciotomy?
Fasciotomy in the limbs is usually performed by a surgeon under general or regional anesthesia. An incision is made in the skin, and a small area of fascia is removed where it will best relieve pressure. Plantar fasciotomy is an endoscopic procedure. The physician makes two small incisions on either side of the heel.
What is a decompression fasciotomy?The definitive surgical therapy for compartment syndrome (CS) is emergent fasciotomy (compartment release). The goal of decompression is restoration of muscle perfusion within 6 hours. Following fasciotomy, fracture reduction or stabilization and vascular repair can be performed, if needed.
Article first time published onWhat are the 4 P's of hourly rounding?
Attention will be focused on the four P’s: pain, peripheral IV, potty, and positioning. Rounds will also include an introduction of the nurse or PCT to the patient, as well as an environmental assessment.
Does hourly rounding reduce falls?
Before hourly rounding, the fall rate on the experimental unit was 3.37/1,000 patient days. The rate decreased to 2.6/1,000 patient days with the hourly rounding implementation. The data demonstrated a 23% reduction in falls which was significant clinically.
What is hourly rounding?
Hourly rounding, as the name implies, is the practice of nurses and unlicensed assistive personnel making scheduled visits to the rooms of hospitalized patients and performing specific nursing interventions every hour. The goal is to improve patient outcomes by addressing their needs in a proactive manner.
Which of the six P's indicates irreversible damage?
If unrecognized or untreated, compartment syndrome can lead to irreversible damage and death of tissue within the compartment and sometimes even more serious conditions, including rhabdomyolysis (the rapid destruction of skeletal muscle) and kidney failure.
What are the 5 P's of musculoskeletal assessment?
Assessment of neurovascular status is monitoring the 5 P’s: pain, pallor, pulse, paresthesia, and paralysis.
Are you awake for a fasciotomy?
What will happen during a fasciotomy? You may be given general anesthesia to keep you asleep and free from pain during surgery. You may instead be given regional anesthesia to numb the surgery area. You will be awake with regional anesthesia, but you should not feel pain.
Who created Ganey survey?
Founded in 1985 by Dr. Irwin Press, PhD. and Dr. Rod Ganey, PhD., their goal is to improve clinical and business outcomes.
What is Cicare service commitment?
CICARE is an evidence-based acronym that creates a standard process for interactions with patients, families, and colleagues. Specifically, with every patient and in every encounter, we commit to: • Connect with Compassion by addressing the patients with their chosen name.
What does the R stand for in CI care?
The C-I-CARE program is designed to establish positive, two-way communication between health care professionals and patients. … R: Respond to patient questions or requests promptly. E: Exit courteously, and always with an explanation of what will come next.
What are the 3 P's of nursing rounds?
All [email protected] students are required to take core courses covering advanced concepts in the “Three Ps” — Advanced Health Assessment (Physical,) Physiology and Pathophysiology, and Pharmacology.
What are the 4 P's nursing?
It’s based on the 4 P’s of nursing: Pain, Potty, Position and Periphery. This is not to be confused with the 4 P’s of marketing: Product, Price, Place and Promotion.
What are the four P's in patient care?
The four Ps (predictive, preventive, personalized, participative) [3] (Box 21.1) represent the cornerstones of a model of clinical medicine, which offers concrete opportunities to modify the healthcare paradigm [4].
Is fasciotomy painful?
Pain usually occurs even at rest and may be worse on movement. Pain is likely to occur after surgery, however in compartment syndrome the pain tends to be severe and out of proportion to the injury. Nerve damage may also make the pain worse, resulting in a burning sensation around the area.
Does fascia grow back?
Fascia doesn’t typically heal in its original configuration. Instead of restoring to its previous flat and smooth texture, fascia may heal into a jumbled clump. Called fascial adhesion, fascia can literally stick to existing muscle or developing scar tissue.
How long is recovery after fasciotomy?
The success of your recovery after compartment syndrome surgery will highly depend on your commitment to your physiotherapy programme as well as the condition of your leg prior to the surgery. Recovery will take up to three months.
What is the most common cause of compartment syndrome?
Causes of compartment syndrome a broken bone or a crush injury – this is the most common cause. a plaster cast or tight bandage being applied to a limb before it has stopped swelling. burns, which can cause the skin to become scarred and tight.
How do you diagnose DX compartment syndrome?
In many cases, a definite diagnosis of compartment syndrome requires direct measurement of pressures inside the body compartment. To do this, a doctor can insert a needle into the area of suspected compartment syndrome while an attached pressure monitor records the pressure.
How do you fix compartment syndrome?
The only option to treat acute compartment syndrome is surgery. The procedure, called a fasciotomy, involves a surgeon cutting open the skin and the fascia to relieve the pressure. Options to treat chronic compartment syndrome include physiotherapy, shoe inserts, and anti-inflammatory medications.
What is four compartment fasciotomy of leg?
The lower leg has four compartments: anterior, lateral, superficial posterior, and deep posterior. The fasciotomy of the lower leg can be done with either a single incision or two incisions.
What are the 4 compartments of lower leg?
The lower leg subdivides into four compartments which are the anterior, lateral, superficial posterior and deep posterior compartments.
Can you get compartment syndrome in the thigh?
Thigh Compartment Syndrome is a devastating lower extremity condition where the osseofascial compartment pressure rises to a level that decreases perfusion to the thigh and may lead to irreversible muscle and neurovascular damage.