What is a Grade 3 Cystocele
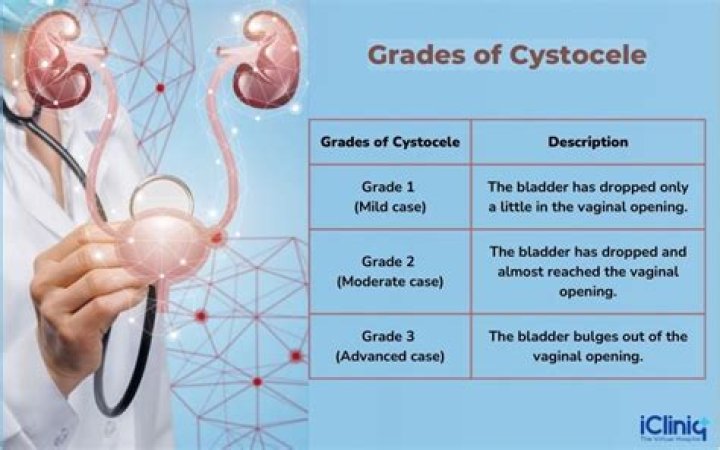
A grade 3 cystocele is the most severe of cystoceles. This is the diagnosis when the bladder droops low enough to bulge completely out of the vagina. Symptoms are similar to those of a grade 2 cystocele—but worse.
How serious is cystocele?
Although not life-threatening, a cystocele can have a negative impact on a woman’s quality of life. If it is not treated at all, the condition can continue to get worse. In the worst cases, the woman may be unable to urinate, which can cause kidney damage or infection.
What is the best treatment for cystocele?
- Kegel exercises (pelvic floor strengthening exercises)
- Physical therapy.
- Vaginal pessary (a vaginal support device)
- Medications such as estrogen replacement therapy.
Can Stage 3 prolapse be reversed?
Yes! Pelvic organ prolapse can be treated and improve without surgery in some women. Prolapse results when the pelvic floor tissues are overstretched and weakened, just like overstretching a spring. Your pelvic floor muscles should work to help support your pelvic organs (i.e. bladder, uterus and rectum).What is a Level 3 prolapse?
Degrees of uterine prolapse Stage I – the uterus is in the upper half of the vagina. Stage II – the uterus has descended nearly to the opening of the vagina. Stage III – the uterus protrudes out of the vagina. Stage IV – the uterus is completely out of the vagina.
What does a cystocele feel like to touch?
Symptoms of cystocele include: Feeling of pelvic heaviness or fullness. Bulge in the vagina that you can feel. Aching or a feeling of pressure in the lower belly or pelvis.
How painful is cystocele surgery?
You may experience discomfort in the vagina for 1-2 weeks following the surgery. The physician may place a medicated vaginal packing in the vagina overnight. The catheter stays for 2-6 days to give the bladder more time to function normally. You may notice bloody discharge and/or odor from the vagina for 1-2 weeks.
Can you push a prolapsed bladder back into place?
If you or your child has a rectal prolapse, you may be able to push the prolapse back into place as soon as it occurs. Your doctor will let you know if this is okay to do.Is walking good for bladder prolapse?
walking – this is the best exercise during bladder prolapse surgery recovery. doing pelvic floor exercises. resting each day.
How many years can you use a pessary?Most vaginal pessaries can be left in for as long as four to six months or unless told otherwise by your healthcare provider. In comparison, a type of pessary used for women with advanced degrees of vaginal prolapse, called cube pessary, should be removed every night.
Article first time published onCan Cystocele repair itself?
When to Seek Medical Care for a Prolapsed Bladder Prolapsed organs cannot heal themselves, and most worsen over time.
Is Cystocele a cause of urinary tract infections?
Defects at any of these levels, and usually a combination of two or all three of them, result in typical anterior compartment prolapse (cystocele), which may predispose to UTIs.
Are Cystocele repairs successful?
Failure rate: None of these procedures has a 100% successful rate. According to studies, 5-15% of women may have to face failure even after a prolapse repair surgery.
Can a Cystocele cause bowel problems?
Constipation. Needing to push organs back up into the vagina to empty the bladder or have a bowel movement. Pain during sex.
Do you have to wear a pessary forever?
Will I have to wear a pessary forever? Pessaries are a safe, long-term management option for pelvic organ prolapse. Some women happily use pessaries for years. Other women choose to just wear their pessary for exercise and physical activity.
How do I know if my prolapse is severe?
- Sensation of heaviness or pulling in your pelvis.
- Tissue protruding from your vagina.
- Urinary problems, such as urine leakage (incontinence) or urine retention.
- Trouble having a bowel movement.
How long is hospital stay after prolapse surgery?
You’ll usually need to stay in hospital overnight or for a few days. Most women can go home once their bladder is emptying well. In rare cases, you may need a catheter for a week or so. You’ll still be able to go home, but you’ll need to come back in a week or two to have the catheter removed.
Are you put to sleep for bladder sling surgery?
You may be given general anesthesia to keep you asleep and free from pain during surgery. You may instead be given anesthesia to numb the surgery area. With this anesthesia, you may still feel pressure or pushing during surgery, but you should not feel any pain.
How long does it take to recover from prolapse bladder surgery?
You can expect to feel better and stronger each day. But you may get tired quickly and need pain medicine for a week or two. You may need about 4 to 6 weeks to fully recover from open surgery and 1 to 2 weeks to recover from laparoscopic surgery or vaginal surgery.
What pessary is used for cystocele?
In patients with a mild cystocele, treatment using a ring with support, a dish with support, a Hodge with support or a donut pessary will suffice. To manage a large prolapse of the anterior vaginal wall, the Gellhorn pessary may be the best choice, although insertion and removal can be difficult.
Can a woman's bladder fall out?
Under normal conditions in women, the bladder is held in place by a “hammock” of supportive pelvic floor muscles and tissue. When these tissues are stretched and/or become weak, the bladder can drop and bulge through this layer and into the vagina. This results in bladder prolapse, also called cystocele.
How do you know if your bladder has fallen?
Patients can usually tell if their bladder has dropped when they face difficulty urinating, pain or discomfort, and stress incontinence (leakage of urine due to exertion or coughing, sneezing, and laughing), which are the most common symptoms of a prolapsed bladder.
How do people live with Cystocele?
- Try Kegel exercises to strengthen your pelvic muscles.
- Achieve and maintain a healthy weight.
- Avoid lifting heavy objects that put stress on pelvic muscles.
- Drink less fluids—no more than 8, 8-ounce cups per day.
- Train your bladder by urinating every 2-3 hours.
Can you use a tampon as a pessary?
Using a tampon instead of a pessary seems like a great fix, with one problem: tampons are not designed to be used as a pessary. They are designed to be absorptive and to expand to fill the vaginal canal as they expand.
What is the success rate of bladder prolapse surgery?
Approximately 94% achieved surgical success when it was defined as the absence of prolapse beyond the hymen. Subjective cure (absence of bulge symptoms) occurred in 92.1% while absence of re-treatment occurred in 97.2% of participants.
Can a prolapse cause a smell?
You may experience pain in your vagina, back or tummy (abdomen). Sometimes, you may also notice a discharge from your vagina, which may be blood-stained or smelly. Sex may be uncomfortable or painful. Symptoms are usually worse after long periods of standing and they improve after lying down.
How do you fix a prolapsed bladder without surgery?
The two non-surgical options for prolapse are pelvic floor muscle training (PFMT) and a vaginal pessary. PFMT can be effective for mild prolapse but is usually not successful for moderate and advanced prolapse. The main alternative to surgery for prolapse is a vaginal pessary.
Does Stage 3 bladder prolapse require surgery?
Grade 3 Cystocele This is the diagnosis when the bladder droops low enough to bulge completely out of the vagina. Symptoms are similar to those of a grade 2 cystocele—but worse. Treatment for this type of bladder prolapse is cystocele repair surgery to move the bladder back into its proper place.
Can I poop with a pessary in?
Pessary use creates the ability for a patient to forgo or to extend their time for a surgical intervention due to pelvic organ prolapse. Looking at the dynamics of the pessary, it may block bowel movement emptying.
Can a pessary go up too far?
The pessary can’t go anywhere else inside the body. However, the pessary can fall out of the vagina if you strain too hard or lift something heavy. This usually means that your pessary is too small. Check with your doctor if your pessary keeps falling out.
What should you not do with a prolapse?
If you have pelvic organ prolapse, avoid things that could make it worse. That means don’t lift, strain, or pull. If possible, try not to be on your feet for long periods of time. Some women find that they feel more pressure when they stand a lot.