What is autocrine gland
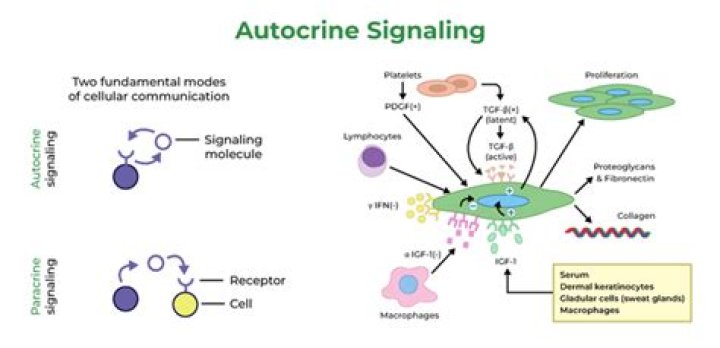
(Autocrine glands are the glands that produce hormones that act on their own glandular cells, e.g., prostaglandins. In contrast, paracrine glands are those whose hormones are released into the extracellular matrix and reach the adjacent cells via diffusion, e.g., islets of Langerhans – somatostatin).
What is an example of autocrine?
Examples. An example of an autocrine agent is the cytokine interleukin-1 in monocytes. When interleukin-1 is produced in response to external stimuli, it can bind to cell-surface receptors on the same cell that produced it.
What is meant by autocrine signaling?
Autocrine signaling means the production and secretion of an extracellular mediator by a cell followed by the binding of that mediator to receptors on the same cell to initiate signal transduction.
What are paracrine glands?
Definition. adjective. Of or relating to a hormone or to a secretion released by (endocrine) cells into the adjacent cells or surrounding tissue rather than into the bloodstream. Supplement.What is autocrine and paracrine?
The main difference between the different categories of signaling is the distance that the signal travels through the organism to reach the target cell. … Paracrine signaling acts on nearby cells, endocrine signaling uses the circulatory system to transport ligands, and autocrine signaling acts on the signaling cell.
Is quorum sensing autocrine?
Quorum sensing involves autocrine cells determining their population den- sity due to the cells engaging in neigh- bor communication without self- communication. the ability of the autocrine cell to achieve self-communication, neighbor communication (including quorum sen- sing), and a mixture of the two.
Is insulin autocrine?
Autocrine signalling involves diffusible molecules that bind to receptors on the same cell from which they have been released. The first transmitter to be implicated in the autocrine regulation of β-cell function was insulin itself.
Is insulin endocrine or paracrine?
Endocrine cells of the pancreas include insulin-secreting beta cells, glucagon-secreting alpha cells, somatostatin-secreting delta cells, and cells that secrete pancreatic polypeptide.How are autocrine and paracrine difference?
The key difference Between Autocrine and Paracrine is that the autocrine refers to the action of hormones or other secretions on the same cells that they secreted while the paracrine refers to the action of hormones or secretions on the cells nearby the production cells.
What is autocrine loop?A type of interaction between growth factors, cytokines and target cells, in which a cell produces the same growth factors and cytokines for which it has receptors, allowing the cell to stimulate itself, as occurs in smooth muscle cell production and IL-1 response.
Article first time published onWhere does autocrine signaling occur?
Autocrine signalling is a type of cell communication, that occurs when the cell secretes a substance that is capable of provoking a reaction in itself. It comes from auto-, a Greek prefix meaning ‘self’. The secreted molecules are known as local mediators, because they only affect cells in their immediate vicinity.
Is EGF autocrine signaling?
Autocrine signaling from Ras may also lead to activity of EGFR-independent signaling pathways that mediate radioresistance. In summary, activated Ras leads to EGFR activity, which, in turn, activates Ras pathways in a positive feedback mechanism for radioresistance.
Is the pancreas autocrine?
The feedback system of the pancreatic islets is paracrine, and is based on the activation and inhibition of the islet cells by the endocrine hormones produced in the islets.
Do pancreatic beta cells have insulin receptors?
The insulin signal transduction pathway in pancreatic β-cells is similar to that in most other cell types (Fig. 1). We do not dispute evidence that insulin receptors are expressed in β-cells. … IRS-2 is critical because it is a highly regulated “gatekeeper” of islet β-cell homeostasis.
What is the normal renal threshold for glucose?
The plasma glucose concentration above which significant glucosuria occurs is called the renal threshold for glucose. Its value is variable, and deviations occur both above and below the commonly accepted “normal” threshold of 180 mg/dl. In diabetic patients, the value is reported to vary from 54 to 300 mg/dl (6–14).
Is quorum sensing autocrine or paracrine?
Quorum sensing involves autocrine cells determining their population density due to the cells engaging in neighbor-communication without self-communication.
Is chemotaxis a quorum sensing?
Such intercellular signalling, known as quorum sensing, allows bacteria to coordinate and synchronize behavioural responses at high cell densities. … Autoaggregation requires motility and is strongly enhanced by chemotaxis to AI-2 at physiological cell densities.
Is quorum sensing a type of phagocytosis?
P. aeruginosa lasI/rhlI quorum sensing genes promote phagocytosis and AQP9 redistribution to the leading and trailing regions in macrophages.
What is autocrine and endocrine?
The main difference between the different categories of signaling is the distance that the signal travels through the organism to reach the target cell. … Paracrine signaling acts on nearby cells, endocrine signaling uses the circulatory system to transport ligands, and autocrine signaling acts on the signaling cell.
What does your pituitary gland control?
The pituitary gland is called the ‘master gland’ as the hormones it produces control so many different processes in the body. … Through secretion of its hormones, the pituitary gland controls metabolism, growth, sexual maturation, reproduction, blood pressure and many other vital physical functions and processes.
What is an example of a paracrine hormone?
Excellent examples of the paracrine actions of hormones are provided by the ovaries and testes. Estrogens produced in the ovaries are crucial for the maturation of ovarian follicles before ovulation. Similarly, testosterone produced by the Leydig cells of the testes acts on adjacent…
Are neurotransmitters paracrine signals?
Interestingly, neurotransmitters initially thought to be present in autonomic axons innervating the islet are also present in endocrine cells of the human islet. These neurotransmitters can thus be released as paracrine signals to help control hormone release.
Does insulin use paracrine signaling?
A series of recent studies in rodents also point out that intraislet glucagon is needed for adequate insulin secretion in vivo (36–38). These studies found that paracrine glucagon stimulates insulin secretion by activating glucagon and GLP-1 receptors on β-cells.
Where does an autocrine hormone work?
Endocrine action: the hormone is distributed in blood and binds to distant target cells. Paracrine action: the hormone acts locally by diffusing from its source to target cells in the neighborhood. Autocrine action: the hormone acts on the same cell that produced it.
Why might a cell use autocrine signaling?
In autocrine signaling, a cell signals to itself, releasing a ligand that binds to receptors on its own surface (or, depending on the type of signal, to receptors inside of the cell). … For instance, autocrine signaling is important during development, helping cells take on and reinforce their correct identities.
What is Juxtacrine communication?
In biology, juxtacrine signalling (or contact-dependent signalling) is a type of cell–cell or cell–extracellular matrix signalling in multicellular organisms that requires close contact. … A communicating junction links the intracellular compartments of two adjacent cells, allowing transit of relatively small molecules.
What hormone controls blood sugar levels?
What is glucagon? Glucagon is a hormone that is involved in controlling blood sugar (glucose) levels. It is produced by the alpha cells, found in the islets of Langerhans, in the pancreas, from where it is released into the bloodstream.
What do pancreatic alpha cells secrete?
The α-cells secrete glucagon as a response to low blood glucose. The major function of glucagon is to release glucose from the glycogen stores in the liver.
What cell produces insulin?
Beta cells make the hormone insulin, which lowers the glucose level. In type 1 diabetes, the body’s immune system mistakenly destroys the beta cells.
How do beta cells release insulin?
Insulin is secreted by the β-cells of the pancreatic islets of Langerhans in response to elevation of the intracellular Ca2+ concentration ([Ca2+]i). This is produced by an influx of extracellular Ca2+ via voltage-dependent Ca2+ channels, whose activity, in turn, is regulated by the β-cell membrane potential.
Does insulin affect beta cells?
Elements of insulin signaling pathways in β-cells are important. The insulin signal transduction pathway in pancreatic β-cells is similar to that in most other cell types (Fig. 1). We do not dispute evidence that insulin receptors are expressed in β-cells.