What is fluoro time
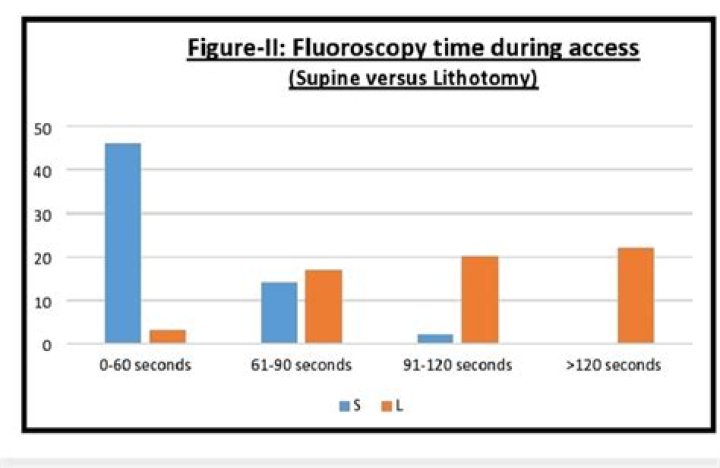
Table 6 lists entrance skin doses for a number of diagnostic procedures, in which the fluoroscopic time typically ranges from ∼3 to 15 minutes (,18,,20,,21) with entrance skin dose ranging from 44 to 340 mGy (4.4–34 rad).
What is the purpose of fluoroscopy?
Fluoroscopy, as an imaging tool, enables physicians to look at many body systems, including the skeletal, digestive, urinary, respiratory, and reproductive systems.
Why is a timer used during fluoroscopic procedures?
Low fluoroscopy times lead to lower patient exposure because there is less “beam on” time. FDA regulations require all fluoroscopy units to be equipped with a timer that alerts the user to excess amounts of fluoroscopy (usually after 4.5 or 5 minutes of use).
What is a Fluoroscan?
Fluoroscans can be thought of as “active x-rays,” allowing patients to view their scans in real-time. Fluoroscopy is an imaging technique that uses low dosages of X-rays to produce moving images of a patient’s internal structures in order to diagnose disease or damage, or to assist during various treatment procedures.How long is fluoroscopy?
This exam is usually completed within 20 minutes. If a Small Bowel Exam is also performed, then the exam could take up to 4hrs.
What is fluoroscopy guidance?
Fluoroscopy is a form of X-ray imaging guidance that helps your doctor to locate the internal injection site where an injection, such as a steroid or joint injection is to be administered for pain relief. Fluoroscopy is like GPS (global positioning system) navigation for the tip of an injection needle.
Why is it called fluoroscopy?
Both live moving images and recorded still images were available from the beginning with simple equipment; thus, both “looking with a fluorescent screen” (fluoro- + -scopy) and “recording/engraving with radiation” (radio- + -graphy) were immediately named with New Latin words—both words are attested since 1896.
How much radiation do you get from fluoroscopy?
Getting a fluoroscopic procedure exposes a patient to as much radiation as 250 to 3,500 chest X-rays. For perspective, a person gets the equivalent of one chest X-ray from normal background radiation in about two and a half days.What is a fluoroscopy Esophagram?
A barium swallow test (cine esophagram, swallowing study, esophagography, modified barium swallow study, video fluoroscopy swallow study) is a special type of imaging test that uses barium and X-rays to create images of your upper gastrointestinal (GI) tract.
Does fluoroscopy require contrast?One common fluoroscopy exam involves a barium (or contrast) swallow, which passes through the GI tract and allows doctors to see the GI movements in even greater detail.
Article first time published onHow much fluoro time is too much?
The skin entrance exposure limitations set by regulatory bodies are 2.58 mC/kg per minute (10 R/min) for normal fluoroscopy and 5.16 mC/kg per minute (20 R/min) for high-dose fluoroscopy. Currently, there are no maximum limitations on other fluoroscopic imaging modes, such as cine and digital subtraction angiography.
What is pulse rate in fluoroscopy?
Normally, fluoroscopy pulse rates of between 7.5 and 15 pulses per second (PPS) are used for coronary angiography and the choice of pulse rate is dependent on the operator’s preference.
What is kVp and mAs in radiology?
* kVp: the power and strength of the x-ray beam (quality of the x-rays). * mAs: the number of x-ray photons produced by the x-ray tube at the setting selected (quantity of x-rays). * time: how long the exposure lasts. Understanding Technique. kVp stands for kilovoltage peak.
Who performs fluoroscopy?
Who performs fluoroscopy? Many types of doctors perform fluoroscopy to diagnose conditions and guide certain treatment procedures, such as a cardiac catheterization. Doctors who commonly use fluoroscopy include: Cardiologists specialize in diagnosing and treating heart diseases.
Is ultrasound a fluoroscopy?
In these procedures, fluoroscopy simply serves as an image-guidance tool, and as such, alternative imaging modalities that do not rely on ionizing radiation can and should be considered. For example, as a real-time, high-resolution imaging modality, ultrasound shares many characteristics with fluoroscopy.
What is fluoroscopy NHS?
Fluoroscopy is an imaging technique used to visualise internal organs in the body whilst they are in motion using x-rays. If an x-ray is a still picture, fluoroscopy is like a movie.
What is the history of fluoroscopy?
Fluoroscopy can be traced back to 1895, when Wilhelm Röntgen noticed a barium platinocyanide screen fluorescing due to exposure to what he would later define as x-rays. … Edison is also credited with creating and designing the first commercially available fluoroscope sometime prior to 1900 [2].
When did fluoroscopy start?
Thomas Alva Edison invented the fluoroscope in 1896, only one year after Wilhelm Conrad Rontgen’s discovery of X rays. The primary function of the fluoroscope is to create images of the internal structures and fluids in the human body.
What's the difference between Cine and fluoroscopy?
Fluoroscopic LFH images conventionally have inferior diagnostic quality when compared with cine coronary angiography, but with new angiographic systems with improved LFH image quality, these images may be adequate for diagnostic coronary angiography.
What is the CPT code 76942?
Description of CPT 76942: The CPT Code 76942 is used for all ultrasonic guided needle placements, including biopsy, aspiration and injection, and is a CPT specific code for ultrasonic guided procedures. This code is not used for vascular surgery.
What are the components of fluoroscopy?
The key components include an X-ray tube, spectral shaping filters, a field restriction device (aka collimator), an anti-scatter grid, an image receptor, an image processing computer and a display device.
What is Esophagram for?
Your doctor has requested a procedure called an esophagram or barium swallow. This exam is performed to assess frequent heartburn (pain), gastric reflux (food/acid coming back up), aspiration (food or fluid in your wind pipe), difficulty eating, drinking, or swallowing.
What happens during an Esophagram?
What Happens During the Test? The patient will drink barium as the radiologist takes x-ray images. For air contrast, you will also be asked to swallow a crystal like substance. These crystals form gas in the stomach, which helps the stomach show up on x-ray.
What does a Esophagram show?
What is it? An esophagram is a radiology study of the esophagus – the part of the body connecting the mouth and stomach. In this exam, barium is used as a contrast agent to assess the anatomy and function of the esophagus with fluoroscopy and x-ray.
What are the risks of fluoroscopy?
- radiation-induced injuries to the skin and underlying tissues (“burns”), which occur shortly after the exposure, and.
- radiation-induced cancers, which may occur some time later in life.
What is the advantage of fluoroscopy?
What are the benefits and risks of fluoroscopy? Medical imaging tests such as fluoroscopy are non-invasive procedures that allow doctors to diagnose diseases and injuries. These tests can help doctors: Obtain a better view of organs, blood vessels, tissues and bones.
How much is a fluoroscopy?
How Much Does Fluoroscopy Cost? On MDsave, the cost of Fluoroscopy ranges from $128 to $1101. Those on high deductible health plans or without insurance can shop, compare prices and save.
What is the difference between fluoroscopy and CT scan?
Overall, fluoroscopy is a safe procedure, but potential risks include burns or radiation-induced injuries to the skin. On the other hand, CT scans are still snapshots of a “slice” of the body. They use X-rays to help your doctor view important organs.
How far does scatter radiation travel?
A general rule of thumb is that the amount of scatter radiation at 1 meter (m) from the side of the patient will be 0.1% of the intensity of the primary x-ray beam.
How far from C arm is safe?
Adjust distance. Your patient’s exposure to radiation increases exponentially by how close the patient is to the x-ray tube. Try to position your patient as far as possible from the tube. Ideally, your patient should be 12-15 inches away.
How much radiation is in a mini C arm?
Results: The mean in-beam radiation exposures with the use of the mini and standard C-arms were 3,720 mR/h and 6,540 mR/h, respectively. The mini C-arm had universally less radiation exposure than the standard C-arm in the clinical configurations tested.