What is the main purpose of the tracheostomy cuff
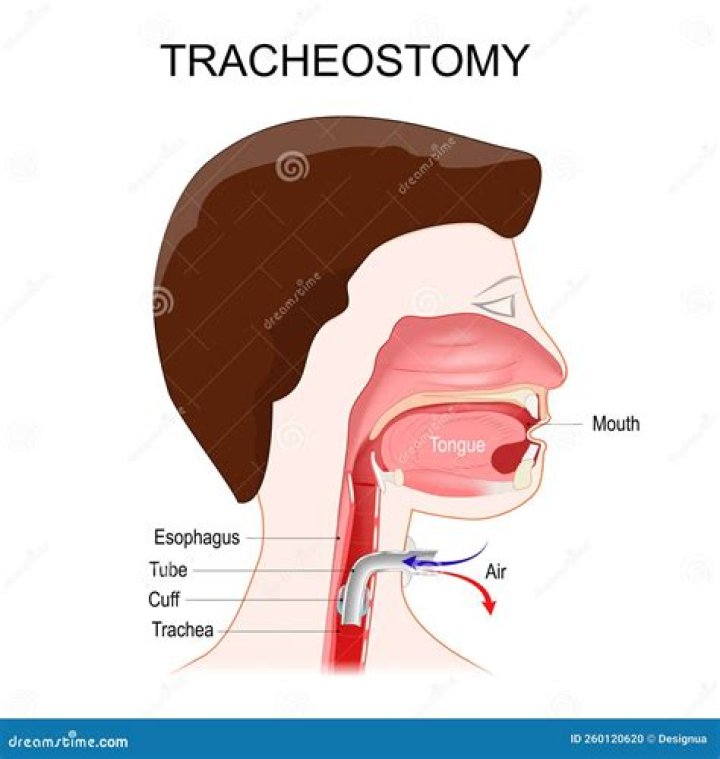
Cuffed tubes allow positive pressure ventilation and prevent aspiration. If the cuff is not necessary for those reasons, it should not be used because it irritates the trachea and provokes and trap secretions, even when deflated.
Which of the following is the function of the cuff in the tracheostomy tube?
Purpose of the tracheostomy cuff The purpose of the cuff is to maintain the air delivered from the mechanical ventilator to the lungs. The cuff fills the tracheal space around the tracheostomy tube to prevent airflow from escaping around the tube and through the upper airway.
What is cuff pressure in tracheostomy?
The cuff pressure is defined as the pressure in the cuff of a tracheal tube, exerted against the mucosal tissue of the trachea to hold the tube in place (Figure 2). The tracheostomy cuff is an inflatable balloon near the end of the tube that creates a seal against the tracheal wall (Figure 3).
Does a cuffed trach prevent aspiration?
The definition of aspiration is when any food, liquid, or other matter passes below the vocal folds. Therefore, the cuff cannot prevent aspiration as it is located below the vocal folds.What type of tracheostomy cuff should be used?
Specific types of cuffs used on tracheostomy tubes include high-volume low-pressure cuffs, tight-to-shaft cuffs (low-volume high-pressure), and foam cuffs. High-volume low-pressure cuffs are most commonly used. Tracheal capillary perfusion pressure is normally 25–35 mm Hg.
What are the complications of over inflating the cuff of a tracheostomy tube?
Complications of cuff over-inflation include: Tracheal stenosis, tracheomalacia, tracheo-esophageal fistula, and tracheo-innominate artery fistula. In addition to increased possibility of airway injury, higher cuff pressures also have a deleterious effect on swallowing.
Why is it important to measure cuff pressures?
The importance of ETT cuff pressures is highlighted by the spectrum of complications that can occur outside the ideal pressure range. High cuff pressures can result in complications ranging from sore throat and hoarseness[16,17] to tracheal stenosis, necrosis, and even rupture[18-21].
When would you use an uncuffed tracheostomy tube?
An uncuffed tube is suitable for a patient in the recovery phase of critical illness who has returned from intensive care and may still require chest physiotherapy, suction via the trachea and airway support.How do you tell if a trach is cuffed or uncuffed?
If the tracheostomy tube has a pilot line and pilot balloon, this is an indicator that the patient has a cuffed tracheostomy tube. The flange of the tracheostomy tube also indicates if the tracheostomy tube has a cuff in place. When the pilot balloon is inflated, this indicates that the cuff is inflated.
What is the ideal cuff pressure?The cuff is inflated to seal the airway to deliver mechanical ventilation. A cuff pressure between 20 and 30 cm H2O is recommended to provide an adequate seal and reduce the risk of complications. Survey results5–7 indicate that cuff pressure is usually monitored and adjusted every 8 to 12 hours.
Article first time published onWhat is a cuff manometer?
From what I understand, a cuff manometer is used to measure the pressure of the cuff on an endotracheal tube. This can be important when ascending in an unpressurized cabin of a non-standard air evacuation platform.
Why would a patient require a tracheostomy tube with an inflated cuff?
A cuff is necessary when a patient is on a mechanical ventilator. Inflating the cuff during mechanical ventilation makes sure that air is entering the lungs and not escaping through the nose and mouth. The cuff also prevents aspiration of saliva in patients who have trouble swallowing.
What is the purpose of an obturator in a tracheostomy?
The obturator is used to insert a tracheostomy tube. It fits inside the tube to provide a smooth surface that guides the tracheostomy tube when it is being inserted.
How often should cuff pressure be measured?
The authors recommended to measure intracuff pressure every 8–24 h because the air inside the cuff may escape from the endotracheal cuff surface or through the pilot balloon valve [56, 57].
How much should a trach cuff be inflated?
How to Inflate Cuff. Measure 5 to 10 mL of air into syringe to inflate cuff. If using a neonatal or pediatric trach, draw 5 ml air into syringe. If using an adult trach, draw 10 mL air into syringe.
Can you swallow with cuff inflated?
While a consensus does not exist in the research, it has been reported that an inflated cuff may impinge upon swallowing by tethering the larynx and reducing hyolaryngeal excursion during the swallow.
What is the difference between cuffed and uncuffed ET tubes?
Cuffed tubes provide a leak-proof connection between the patient’s lung and the bag or ventilator without causing undue pressure to laryngeal or tracheal structures [17]. However, an uncuffed endotracheal tube usually causes air leakage or laryngeal injury.
How do you control a cuff?
- Stay hydrated: Drink lots of water to thin mucus.
- Inhale steam: Take a hot shower, or boil water and pour into a bowl, face the bowl (stay at least 1 foot away), place a towel over the back of your head to form a tent and inhale. …
- Use a humidifier to loosen mucus.
What is an airway cuff?
The cuff of the endotracheal tube (ETT) is designed to provide a seal within the airway, allowing airflow through the ETT but preventing passage of air or fluids around the ETT.
What device measures cuff pressure?
Cuff pressures were measured using aneroid manometer. ETT cuff pressure of 20–30 cm of water was considered as standard.
Can you eat with a cuffed tracheostomy?
Most people with a tracheostomy tube will be able to eat normally. However, it may feel different when you swallow foods or liquids.
Does a fenestrated trach have a cuff?
This will allow the passage of air through the fenestrations as well as around the tracheostomy tube. There are also uncuffed, fenestrated tracheostomy tubes, which do not have a cuff in place. Uncuffed, fenenestrated tracheostomy tubes allow for the most airflow through the upper airway with the least resistance.
What is the difference between Shiley and Portex?
It can be seen that the nomenclature differs between different brands, for example, Portex™ tubes have ‘sizes’ equal to the ID of the tube without its inner cannula, while the given ‘size’ of Shiley™ tubes does not equate to any measurement, but closely approximates to the ID of the inner cannula (which must be in …
What is the difference between proximal and distal Trachs?
Proximal vs distal extended length Proximal extended length refers to distance between flange and bend. Distal extended length refers to distance after bend to tip of tube.



