Which is a contraindication for use of peritoneal dialysis
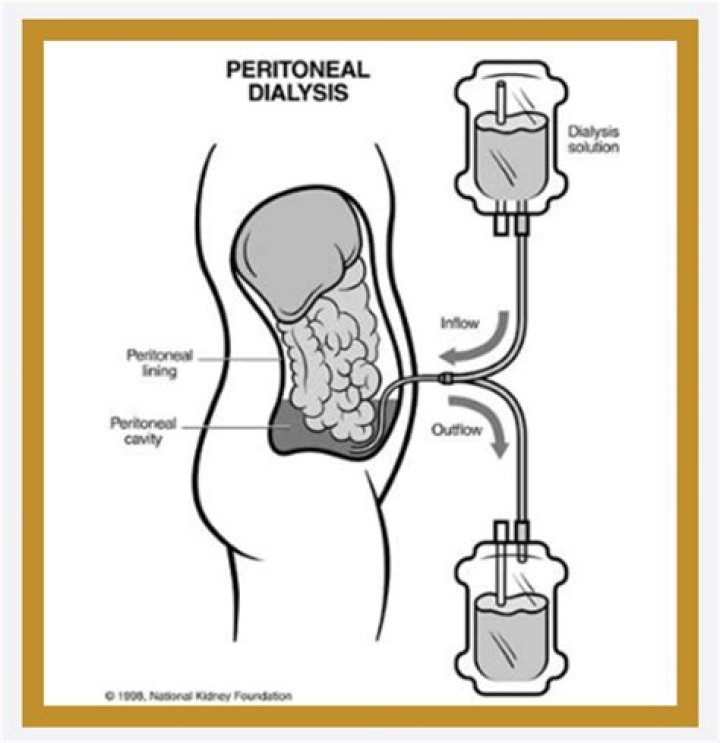
Clinical contraindications include inflammatory abdominal processes such as Crohn disease, ulcerative colitis, current clostridium difficile infection, and end-stage liver disease with ascites. The main anatomic contraindication to PD is an unrepaired hernia that would potentially increase in size with the use of PD.
Is peritonitis contraindication for peritoneal dialysis?
Absolute contraindications for PD are the following: recent abdominal or cardiothoracic surgery, diaphragmatic peritoneal-pleural connections, faecal or fungal peritonitis. Other contraindications are relative.
Is colostomy a contraindication to peritoneal dialysis?
BELIEF: Patients with an ostomy can’t do PD. FACT: Although there are concerns about leaks and catheter or exit site infection from urine or feces contamination, one study found reasonable outcomes for PD in patients with ostomies.
Which one is not an absolute contraindication for peritoneal dialysis?
Relative contraindications for PD include patients with severe malnutrition, multiple abdominal adhesions, ostomies, proteinuria >10 g/day, advanced COPD, ascites, presence of a Le Veen or ventriculo-peritoneal shunt, upper limb amputation with no help at home, poor hygiene, dementia, and those who are homeless.Is cirrhosis a contraindication to peritoneal dialysis?
In older textbooks the use of peritoneal dialysis (PD) in patients with liver cirrhosis and/or ascites was contraindicated.
What is a common problem with peritoneal dialysis?
Infections. The most common problem for people receiving peritoneal dialysis is peritonitis, an infection of the lining of the abdominal cavity (peritoneum). An infection can also develop at the site where the tube (catheter) is inserted to carry the cleansing fluid into and out of your abdomen.
What are complications of peritoneal dialysis?
- Infections. An infection of the abdominal lining (peritonitis) is a common complication of peritoneal dialysis. …
- Weight gain. The dialysate contains sugar (dextrose). …
- Hernia. Holding fluid in your abdomen for long periods may strain your muscles.
- Inadequate dialysis.
What are the contraindications of hemodialysis?
- Difficult vascular access.
- Needle phobia.
- Cardiac failure.
- Coagulopathy.
Is obesity a contraindication for peritoneal dialysis?
Some view obesity as an absolute or relative contraindication to peritoneal dialysis (PD), with the main concerns being metabolic complications, infectious complications, PD fluid leaks, lower dialysis adequacy, and lower patient survival.
What is Haemodialysis and peritoneal dialysis?There are two kinds of dialysis. In hemodialysis, blood is pumped out of your body to an artificial kidney machine, and returned to your body by tubes that connect you to the machine. In peritoneal dialysis, the inside lining of your own belly acts as a natural filter.
Article first time published onWhat causes stoma?
There are many reasons why you may need a stoma. Common reasons include bowel cancer, bladder cancer, inflammatory bowel disease (Crohn’s Disease or Ulcerative Colitis), diverticulitis or an obstruction to the bladder or bowel. A stoma can be temporary or permanent depending on the cause.
What are the different types of peritoneal dialysis?
Share: There are 2 types of peritoneal dialysis (PD): continuous ambulatory peritoneal dialysis (CAPD) and automated peritoneal dialysis (APD). Both types of PD have slightly different advantages, so it really comes down to your personal preference and schedule along with your nephrologist’s recommendation.
When is hemodialysis used?
When is dialysis needed? You need dialysis if your kidneys no longer remove enough wastes and fluid from your blood to keep you healthy. This usually happens when you have only 10 to 15 percent of your kidney function left. You may have symptoms such as nausea, vomiting, swelling and fatigue.
Can you do peritoneal dialysis with ascites?
Peritoneal dialysis (PD) can be an ideal treatment in cirrhotic patients with ascites and chronic kidney disease stage 5 (CKD 5D) who require dialysis.
What is recurrent ascites?
Refractory ascites is defined as ascites that does not recede or that recurs shortly after therapeutic paracentesis, despite sodium restriction and diuretic treatment. To date, there is no approved medical therapy specifically for refractory ascites.
What is Nephrogenic ascites?
Nephrogenic ascites is an entity that manifests as refractory ascites in patients with end-stage renal disease, where portal hypertensive, infectious, and malignant processes have been excluded. Most of these patients are undergoing hemodialysis.
What is the most frequent complication of peritoneal dialysis?
The most frequent and important complication of peritoneal dialysis (PD) catheters is infection, which may result in catheter loss and discontinuation of PD [1,2].
What are the principles for administering peritoneal dialysis?
The principles of peritoneal dialysis are based on the physiological processes and their driving forces which permit the exchange of water (by ultrafiltration and fluid absorption) and solutes (by diffusion and convective transport) between the peritoneal microvasculature and the dialysate.
Why is heparin used in peritoneal dialysis?
Heparin (Heparin Sodium) is a medicine that prevents clots (anticoagulant). It may be used to prevent fibrin formation associated with peritoneal dialysis.
What is hemoperfusion system?
Hemoperfusion refers to the circulation of anticoagulated blood through an extracorporeal circuit with a disposable, adsorbent-containing cartridge (typically activated charcoal or an exchange resin).
What causes fibrin to form in peritoneal dialysis patients?
Questions About PD “Fibrin occurs as a result of protein formation from fibrinogen in the blood…. Strands of fibrin lead to poor drainage (i.e. inflow and outflow) and is usually seen in the outflow bag as pieces of cotton wool.” (page 293). From Oxford Handbook of Renal Nursing (2013), Oxford University Press.
Who is not a candidate for hemodialysis?
Dialysis may not be the best option for everyone with kidney failure. Several European studies have shown that dialysis does not guarantee a survival benefit for people over age 75 who have medical problems like dementia or ischemic heart disease in addition to end-stage kidney disease.
What are the indications for emergent dialysis?
- Acid-base disturbance: acidemia e.g. Severe metabolic acidosis (pH <7.1)
- Electrolyte disorder: usually hyperkalemia; sometimes hypercalcemia, tumor lysis.
- Intoxication: methanol, ethylene glycol, lithium, salicylates.
- Overload of volume (CHF); fluid overload.
What is a common side effect for hemodialysis?
A drop in blood pressure is a common side effect of hemodialysis. Low blood pressure may be accompanied by shortness of breath, abdominal cramps, muscle cramps, nausea or vomiting.
Which is safer hemodialysis or peritoneal dialysis?
Summary: PD is a safe and effective option for patients with kidney failure who need dialysis. It offers several advantages over in-center hemodialysis and may be the right option for many people.
What is the primary disadvantage of using peritoneal dialysis for long term management of chronic renal failure?
One of the main disadvantages of peritoneal dialysis is that it needs to be carried out every day, which you may find disruptive. You may also find it upsetting to have a thin tube (catheter) left permanently in your abdomen (tummy), although it can often be concealed under clothing.
What is in peritoneal dialysis solution?
During PD, a mixture of dextrose (sugar), salt, and other minerals dissolved in water, called dialysis solution, is placed in a person’s abdominal cavity through a catheter.
What are the three major problems associated with having a stoma?
Common complications include poor stoma siting, high output, skin irritation, ischemia, retraction, parastomal hernia (PH), and prolapse. Surgeons should be cognizant of these complications before, during, and after stoma creation, and adequate measures should be taken to avoid them.
What are the 3 types of ostomy?
There are different types of ostomies. The three most common ones are colostomy, ileostomy, and urostomy. Each ostomy procedure is done for different reasons.
What are the factors to consider in deciding to undergo colostomy?
- Infection of the abdomen, such as perforated diverticulitis or an abscess.
- Injury to the colon or rectum (for example, a gunshot wound).
- Partial or complete blockage of the large bowel (intestinal obstruction).
- Rectal or colon cancer.
- Wounds or fistulas in the perineum.
What is the most common complication of AV fistula?
Heart failure. This is the most serious complication of large arteriovenous fistulas. Blood flows more quickly through an arteriovenous fistula than it does through normal blood vessels. As a result, your heart pumps harder to make up for the increase in blood flow.