Who qualifies for Husky B
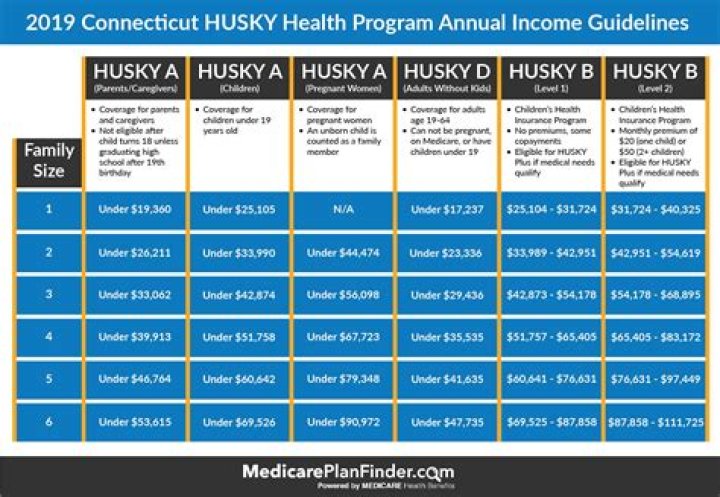
HUSKY B provides medically necessary health care coverage including prescription, dental, and mental health coverage, for uninsured children under age 19 who do not qualify for HUSKY A (Medicaid). HUSKY B also provides intensive care management services for children with special health care needs.
What is Husky B coverage?
HUSKY B provides medically necessary health care coverage including prescription, dental, and mental health coverage, for uninsured children under age 19 who do not qualify for HUSKY A (Medicaid). HUSKY B also provides intensive care management services for children with special health care needs.
What is the income limit for Husky C in CT?
HUSKY C Medicaid for Employees with Disabilities The income limit for these individuals is $75,000. The asset limit for a single adult is $10,000 and $15,000 for a married couple. Visit CT.gov for more information and to apply or call 1-800-537-2549 (Toll-Free).
Do I have Husky A or B?
To see whether you belong to HUSKY A, B, C or D, simply look at your HUSKY ID Card. The big, bold letter is your HUSKY program. HUSKY Health Member Handbooks give you details on your medical benefits and services.What is the income limit for Access Health CT?
For qualifying residents above 400% of the federal poverty level (income of $51,040 for one person), their annual contributions will be capped at 8.5% beginning in May. A presentation by Access Health CT shows examples of how the new subsidies will affect households of different sizes and income levels.
Do you have to pay back Husky insurance?
If a person is aged 55 and older, the state can recover the cost of any medical care that was covered by HUSKY D. The state would seek repayment from the estate of the person when he or she dies, but not while the person is alive, according to the state Department of Social Services.
Is Husky a qualified health plan?
Types of coverage HUSKY and Qualified Health Plans are two forms of health coverage. HUSKY is the state’s public health coverage program. It provides coverage for individuals who qualify based on factors like income and household composition. There are three types of HUSKY: A, B, C, and D.
Who is eligible for the CHIP program?
To be eligible for this benefit program, applicants must live in the state in which they apply and meet all of the following: Either 18 years of age and under or a primary care giver with a child(ren) 18 years of age and under, and. A U.S. Citizen, National, or a Non-Citizen legally admitted into the U.S, and.What is husky C?
What is HUSKY C? HUSKY C – a medicaid plan,is part of the Connecticut State’s HUSKY Health coverage program.It provides health coverage for eligible adults 65 and older and adults with disabilities,and for Employees with Disabilities.
Is a newborn baby covered under Mother insurance?Yes, regardless of whether you have an individual or family health insurance plan, your newborn will be covered for the first 30 days of life. At this time, nothing about your policy or deductible will change as checkups and other care for your baby are included within the mother’s coverage.
Article first time published onHow do you prove income for health insurance?
- Pay stub.
- Bank Statements (personal & business)
- Copy of last year’s federal tax return.
- Wages and tax statement (W-2 and/ or 1099)
What is qualified health plan?
As defined in the Affordable Care Act (ACA), a QHP is an insurance plan that is certified by the Health Insurance Marketplace, provides essential health benefits (EHBs), follows established limits on cost sharing, and meets other requirements outlined within the application process. …
What is a qualified health plan CT?
Qualified Health Plan (QHP) An insurance plan that is certified by Access Health CT, provides Essential Health Benefits, follows established limits on cost -sharing (like deductibles, co-payments, and out-of-pocket maximum amounts), and meets other requirements.
How does insurance work if you lose your job?
If you leave your job for any reason and lose your job-based insurance, you can buy a Marketplace plan. Losing job-based coverage, even if you quit or get fired, qualifies you for a Special Enrollment Period any time to enroll in coverage for the rest of the year.
Can you get Obamacare between jobs?
Can I get health insurance after quitting a job? Yes, you can still get health insurance if you quit your job. You can keep your job-based coverage for up to 18 months with a COBRA plan. Or you can buy an individual plan through the Health Insurance Marketplace.
What factors are used to determine if you qualify for Medicaid and CHIP?
Medicaid eligibility depends on several factors including a consumer’s income level, the number of people in their household, their citizenship or immigration status, and the state in which they live. Some consumers may be eligible if they are disabled, pregnant, or have certain medical needs.
Does my kid qualify for CHIP?
In order to be eligible for CHIP, a child must be: Under 19 years of age, … Eligible within the state’s CHIP income range, based on family income, and any other state specified rules in the CHIP state plan.
Is CHIP and Medicaid the same thing?
Medicaid is intended to provide care for the poorest children. The CHIP program was established in 1997 as a way to expand coverage to children who have lower family incomes but who fall outside the Medicaid eligibility window. … 5 CHIP can also cover care for pregnant women but that coverage is more variable.
What is the 48 96 hour rule?
If you deliver in the hospital, the 48-hour period (or 96-hour period) starts at the time of delivery. So, for example, if a woman goes into labor and is admitted to the hospital at 10 p.m. on June 11, but gives birth by vaginal delivery at 6 a.m. on June 12, the 48-hour period begins at 6 a.m. on June 12.
Can I use my boyfriends insurance for pregnant?
Unfortunately, the answer is likely “no.” Most insurance plans require that you’re married in order to include a partner under your coverage, with some states providing exceptions for common law marriages.
What happens if you forget to add baby to insurance?
If your baby goes even one day without coverage between being on the mother’s insurance and being added to his or her own insurance plan, you could be subject to an additional 20% cost penalty during the first year of your baby’s health insurance coverage — which is already the most expensive year for health insurance.
How do I get self employed medical?
Generally, if you run your own business and have no employees, or are self-employed, your business won’t qualify for group coverage. You can purchase qualified health coverage through the Marketplace for individuals and families. With an Individual Marketplace plan, you can: Find coverage for yourself and your family.
What can proof of income be?
The most common documentation for proof of income includes: Pay stub. Bank Statements (personal & business) Copy of last year’s federal tax return. Wages and tax statement (W-2 and/ or 1099)
How do I figure out what my annual income is?
Multiply the number of hours you work per week by your hourly wage. Multiply that number by 52 (the number of weeks in a year). If you make $20 an hour and work 37.5 hours per week, your annual salary is $20 x 37.5 x 52, or $39,000.
How do I become a qualified health plan?
Have been certified by the Federally Facilitated Marketplace (FFM) Provide coverage of essential health benefits; Follow established limits on cost-sharing (like deductibles, copayments, and out-of-pocket maximum amounts); and.
What does not make a health plan qualified?
A primary example of a “non-qualified health plan” is an employer-sponsored policy. . Grandfathered and grandmothered health insurance plans – which pre-date the ACA and meet some, but not all ACA requirements – are also examples of non-qualified health plans.
What is a non-qualified health plan?
A non-qualified plan is any medical plan that does not meet HDHP requirements. Coverage under any other medical plan (primary or secondary/dependent coverage) will make you ineligible for an HSA plan. … Some plans cover spouses by default and could make you ineligible to contribute to an HSA plan.
What is qualified health plan without financial assistance?
QHPs are plans for individuals and families who have an income that makes them ineligible for a public program, such as MinnesotaCare or Medical Assistance. All QHP plans meet the minimum essential benefits requirement, and some consumers can even qualify for tax credits and cost sharing.
What is a qualified health professional?
A “physician or other qualified health care professional” is an individual who is qualified by education, training, licensure/regulation (when applicable), and facility privileging (when applicable) who performs a professional service within his/her scope of practice and independently reports that professional service. …
What does Qualified health plan with tax credits mean?
Under the Affordable Care Act (ACA), the designation of qualified health plan (QHP) is given to health insurance plans that are sold in the government-run marketplace (exchange). … A qualified health plan is also eligible to be purchased with an advanced premium tax credit, also known as an Obamacare subsidy.
How long after losing job does insurance last?
If you lose your job, you may have the right to continue your health insurance coverage for 18 months—but you’ll have to pay the full premium.