Why is inulin administration an effective way of measuring renal clearance rates
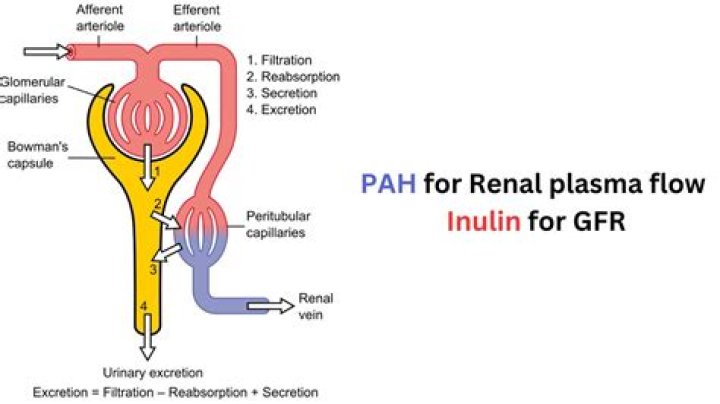
Why is inulin administration an effective way of measuring renal clearance rates? Inulin is filtered and completely reabsorbed in the distal tubule. … When the macula densa detects an increase in NaCl concentration in the renal filtrate, what happens to the glomerular filtration rate (GFR)? GFR decreases.
When the plasma concentration of a substance exceeds its renal threshold?
glucose secretion. When the plasma concentration of a substance exceeds its renal concentration, more of the substance will be ANSWER: excreted.
Which of the following conditions would cause an increase in the glomerular filtration rate GFR?
Glomerular filtration is occurs due to the pressure gradient in the glomerulus. Increased blood volume and increased blood pressure will increase GFR.
When the macula densa detects an increase in sodium chloride concentration in the renal filtrate What happens to the glomerular filtration rate?
As part of the body’s blood pressure regulation, the macula densa monitors filtrate osmolarity; if it falls too far, the macula densa causes the afferent arterioles of the kidney to dilate, thus increasing the pressure at the glomerulus and increasing the glomerular filtration rate.Which kidney process is always active and always requires energy to occur?
The kidneys do not reabsorb filtered waste products. Which of the following kidney processes is always active and always requires energy to occur? proximal tubule.
What is a renal threshold and why is it important?
We defined the renal threshold for glucose reabsorption as the lowest blood glucose level that correlated with the first detectable appearance of urine glucose.
Why is renal threshold important?
The importance of renal threshold in the interpretation of urine tests is shown by the association we have observed be- tween the mean blood glucose achieved by the patients and the level of their renal threshold.
How does macula densa increase GFR?
Reduced NaCl uptake via the NKCC2 at the macula densa leads to increased renin release, which leads to restoration of plasma volume, and to dilation of the afferent arterioles, which leads to increased renal plasma flow and increased GFR.Why is inulin an exogenous substance useful in determining glomerular filtration rate GFR )?
Why is inulin, an exogenous substance, useful in determining glomerular filtration rate (GFR)? … Inulin is secreted from the peritubular fluid into the lumen of the renal tubule. Inulin’s filtered load is greater than its excretion rate. Inulin is freely filtered and not reabsorbed or secreted.
What is the function of the macula densa quizlet?The macula densa cells monitor the NaCl content of the filtrate entering the distal convoluted tubule.
Article first time published onHow does renal blood flow affect GFR?
Because renal blood flow and GFR normally change in parallel, any increase in renal blood flow causes an increase in GFR. The increased renal O2 consumption (GFR) is offset by an increase in renal oxygen delivery (renal blood flow). This results in a constant arteriovenous O2 difference across the kidney.
Why does GFR increase in pregnancy?
Hormonal changes during pregnancy allow for increased blood flow to the kidneys and altered autoregulation such that glomerular filtration rate (GFR) increases significantly through reductions in net glomerular oncotic pressure and increased renal size.
How does high blood pressure affect GFR?
Hypertension is one of the most important causes of end-stage renal disease, but it is unclear whether elevated blood pressure (BP) also accelerates the gradual decline in the glomerular filtration rate (GFR) seen in the general population with increasing age.
Why do patients taking loop diuretics need to take supplemental potassium?
Diuretics inhibit chloride-associated sodium reabsorption in the kidney, creating a favorable electrochemical gradient for potassium secretion.
Which kidney process is mostly active and usually requires energy to move solutes?
Active transport This process requires energy to move solutes against their concentration gradient. Primary active transport relies on energy from the breakdown of adenosine tri-phosphate (ATP) to power a cell membrane protein which ‘pumps’ solutes across a cell membrane.
Which of the following are functions of the kidney quizlet?
- regulate H20 balance, ion balance, and acid-base balance.
- removal of metabolic waste from blood, secretion in urine.
- removal and excretion of foreign toxins.
- gluconeogenesis.
- production of hormones/enzymes: EPO, renin, vitamin D conversion to active form.
What is renal threshold value?
The plasma glucose concentration above which significant glucosuria occurs is called the renal threshold for glucose. Its value is variable, and deviations occur both above and below the commonly accepted “normal” threshold of 180 mg/dl. In diabetic patients, the value is reported to vary from 54 to 300 mg/dl (6–14).
How does the renal threshold for glucose relate to the blood glucose level?
The renal threshold for glucose (RTg) corresponds to a blood glucose level of ~180 mg/dL; however, in hospitals, patients are often encountered who are hyperglycemic, but urine glucose test strip‐negative, who remain negative for urine glucose even at blood glucose concentrations >180 mg/dL, implying a high RTg value.
What happens above the renal threshold for glucose?
When the PG concentration exceeds the renal threshold for glucose (e.g., more glucose is filtered by the glomerulus than can be reabsorbed by the renal tubules), glycosuria results. Because of the resulting elevated urine osmolality, a diuresis ensues that is clinically evident as polyuria (increased urination).
How renal function test is done?
Your kidney numbers include 2 tests: ACR (Albumin to Creatinine Ratio) and GFR (glomerular filtration rate). GFR is a measure of kidney function and is performed through a blood test. Your GFR will determine what stage of kidney disease you have – there are 5 stages.
Which of the following are high threshold substances that are reabsorbed completely?
Glucose, sodium and calcium.
What is the difference between transport maximum and renal threshold?
The main reason for the difference between the levels of transport maximum and threshold is that some nephrons excrete glucose in a lower than transport maximum level, and the transport maximum for the kidneys is reached when all the nephrons reach their maximal capacity to reabsorb glucose.
How is inulin tested for kidney function?
inulin clearance, procedure by which the filtering capacity of the glomeruli (the main filtering structures of the kidney) is determined by measuring the rate at which inulin, the test substance, is cleared from blood plasma.
What is the function of inulin?
Overview. Inulin is a type of prebiotic. It’s not digested or absorbed in the stomach. It stays in the bowel and helps certain beneficial bacteria to grow.
What does inulin measure?
Inulin and its analog sinistrin are used to help measure kidney function by determining the glomerular filtration rate (GFR), which is the volume of fluid filtered from the renal (kidney) glomerular capillaries into the Bowman’s capsule per unit time.
How does the macula densa autoregulation the glomerular filtration rate?
Swelling of the macula densa cells signals constriction of the nearby afferent arteriole so that the glomerular filtration of the same nephron is decreased. … The thick ascending limb of the nephron regulates its own single nephron GFR (SNGFR). Figure 7.6.
What is the role of the macula densa?
Macula densa (MD) cells are chief cells within the kidney, playing key sensory and regulatory functions in the maintenance of body fluid, electrolyte homeostasis, and blood pressure.
How does the macula densa autoregulation the glomerular filtration rate if it decreases lower than normal?
The macula densa responds by decreasing ATP release, and there is a subsequent decrease in calcium from the smooth muscle cells of the afferent arteriole. The ensuing result is vasodilation, and increased renin release in an attempt to increase GFR.
What is the function of the macula densa cells of the Juxtaglomerular?
It is located near the vascular pole of the glomerulus and its main function is to regulate blood pressure and the filtration rate of the glomerulus. The macula densa is a collection of specialized epithelial cells in the distal convoluted tubule that detect sodium concentration of the fluid in the tubule.
Which is a function of the macula densa cells of the Juxtaglomerular complex?
Macula densa cells in the distal nephron, according to the classic paradigm, are salt sensors that generate paracrine chemical signals in the juxtaglomerular apparatus to control vital kidney functions, including renal blood flow, glomerular filtration, and renin release.
What is the function of the macula densa cells of the Juxtaglomerular Complex JGC )?
What is the function of the macula densa cells of the juxtaglomerular complex (JGC)? The macula densa cells monitor the NaCl content of the filtrate entering the distal convoluted tubule.