Why Is Spinal contraindicated in aortic stenosis
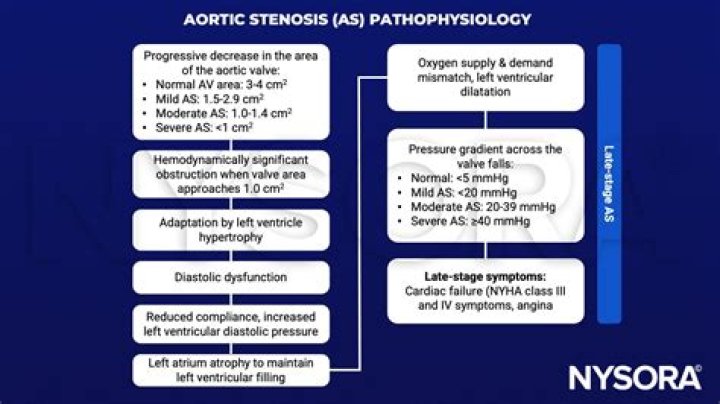
Since patients with SAS have limited stroke volume, any major reduction in systemic vascular resistance may result in sudden fall in perfusion pressure; therefore, spinal anesthesia in patient with aortic stenosis (AS) should be avoided.
Why Is Spinal Anaesthesia contraindicated in aortic stenosis?
The use of central regional anaesthesia is traditionally regarded as contraindicated in patients with severe aortic stenosis due to its sympatholytic effect, potentially causing loss of vascular tone and ultimately diminished cardiac output.
Why ACE inhibitors are contraindicated in aortic stenosis?
There is particular concern that vasodilators may lead to a reduction of the coronary perfusion pressure. In fact, the use of ACE-Inhibitors in aortic stenosis is classically considered to be contraindicated (3).
Is neuraxial blockade contraindicated in the patient with aortic stenosis?
Traditionally, neuraxial blockade has been considered contraindicated in these pa- tients because the sudden and potentially profound decrease in systemic vascular resistance may pre- cipitate life-threatening compromise in coronary perfusion.What can make aortic stenosis worse?
Many of the things that increase the risk of atherosclerosis and heart disease are the same for aortic valve stenosis. They include smoking, high cholesterol, high blood pressure, diabetes, and being male. Birth defect.
How does aortic stenosis cause syncope?
Syncope. Syncope from aortic stenosis often occurs upon exertion when systemic vasodilatation in the presence of a fixed forward stroke volume causes the arterial systolic blood pressure to decline. It also may be caused by atrial or ventricular tachyarrhythmias.
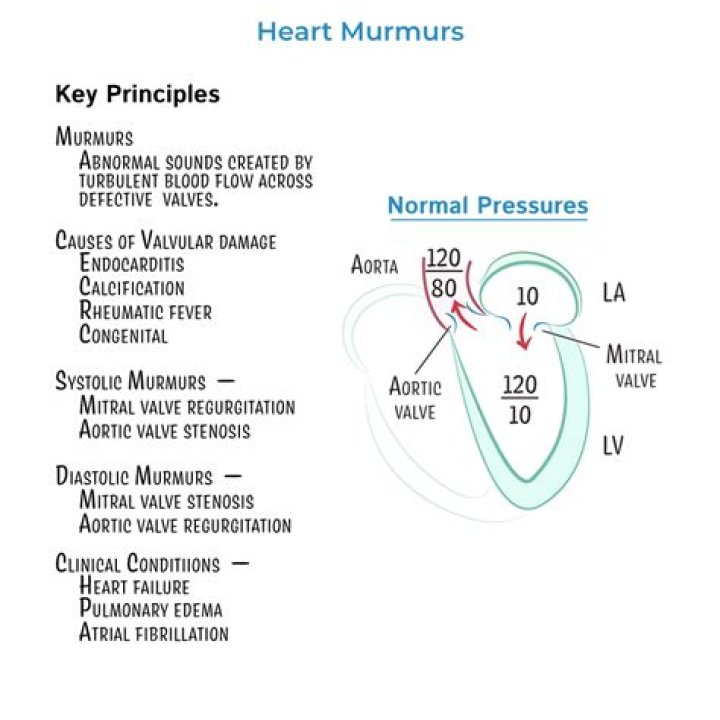
Which manifestations are associated with severe aortic stenosis?
- Abnormal heart sound (heart murmur) heard through a stethoscope.
- Chest pain (angina) or tightness with activity.
- Feeling faint or dizzy or fainting with activity.
- Shortness of breath, especially when you have been active.
Can aortic stenosis cause sudden death?
The incidence of sudden death in asymptomatic patients with severe aortic stenosis might be higher than that reported in previous studies. The cumulative 5‐year incidence of sudden death censored at aortic valve replacement, accounting for the competing risk, was 7.2% (1.4%/year) in asymptomatic patients.What is central regional Anaesthesia?
Central regional blocks were used for surgical anesthesia in 20-40% of reported surgical procedures. Subarachnoid anesthesia was the main technique for orthopedic surgery on the lower limb, elective cesarean section and transurethral resection of the prostate.
What medications should be avoided with aortic stenosis?The patient with severe aortic stenosis is relatively “afterload fixed and preload dependent” — meaning cardiac output does not increase with after-load reduction. Thus all afterload reducing agents (angiotensin-converting enzyme inhibitors, calcium channel blockers, blockers) are contraindicated.
Article first time published onWhy are beta blockers avoided in aortic stenosis?
Background. Patients with aortic stenosis ( AS ) often have concomitant hypertension. Antihypertensive treatment with a β‐blocker (Bbl) is frequently avoided because of fear of depression of left ventricular function.
Is Amlodipine contraindicated in aortic stenosis?
Amlodipine is contraindicated in patients with known hypersensitivity to amlodipine or its dosage form components. In addition, amlodipine is relatively contraindicated in patients with cardiogenic shock, severe aortic stenosis, unstable angina, severe hypotension, heart failure, and hepatic impairment.
How do you prevent aortic stenosis from getting worse?
- Control risk factors. …
- Get regular checkups. …
- Control risk factors. …
- Monitor your symptoms. …
- See your doctor regularly. …
- Transcatheter Aortic Valve Implantation. …
- Surgical Aortic Valve Replacement. …
- Deciding Between TAVI and SAVR.
What is the most common cause of aortic stenosis?
The most common cause of aortic stenosis is the accumulation of calcium deposits on the aortic valve, which increases with age. This causes the aortic valve to stiffen and narrow over time.
What are the end stages of aortic stenosis?
If left untreated, severe aortic stenosis can lead to heart failure. Intense fatigue, shortness of breath, and swelling of your ankles and feet are all signs of this. It can also lead to heart rhythm problems (arrhythmias) and even sudden cardiac death.
What are the triad signs of aortic stenosis?
- Chest pain: Angina pectoris in patients with aortic stenosis is typically precipitated by exertion and relieved by rest.
- Heart failure: Symptoms include paroxysmal nocturnal dyspnea, orthopnea, dyspnea on exertion, and shortness of breath.
Which of the following symptoms of aortic stenosis has the poorest prognosis?
In general, the presence of low-gradient “severe stenosis” (defined as aortic valve area < 1.0 cm2 and mean gradient 40 mmHg), representing up to 40% of all patients with aortic stenosis, is considered to be associated with a poor prognosis.
What compensatory mechanism occurs in the heart in patients suffering from hypertension or aortic valve stenosis that helps to maintain cardiac output?
To compensate for the increasing resistance at the aortic valve, the muscles of the left ventricle thicken to maintain pump function and cardiac output. This muscle thickening causes a stiffer heart muscle which requires higher pressures in the left atrium and the blood vessels of the lungs to fill the left ventricle.
Does aortic regurgitation cause syncope?
Symptoms of aortic regurgitation include: Angina (chest pain) Syncope (fainting) Heart palpitations, which can be caused by rhythm disorders (cardiac arrhythmias)
Is syncope a symptom of severe aortic stenosis?
Alongside dyspnea and angina, syncope is one of the classic cardinal symptoms of severe aortic stenosis (AoS).
What is the pathophysiologic mechanism by which aortic stenosis causes angina pectoris?
The pathophysiology of cardiac pain in pure aortic stenosis has primarily been ascribed to an augmented left ventricular demand outstripping energy supply.
Is spinal anesthesia a regional anesthesia?
Regional anesthesia makes a specific part of the body numb to relieve pain or allow surgical procedures to be done. Types of regional anesthesia include spinal anesthesia (also called subarachnoid block), epidural anesthesia, and nerve blocks.
What is the difference between spinal and regional anesthesia?
Regional anesthesia numbs a larger (but still limited) part of the body and does not make the person unconscious. Sometimes medicine is added to help the person relax or fall asleep. Spinal and epidural anesthesia are examples of regional anesthesia.
What is spinal anesthesia?
Spinal anesthesia is a neuraxial anesthesia technique in which local anesthetic is placed directly in the intrathecal space (subarachnoid space). The subarachnoid space houses sterile cerebrospinal fluid (CSF), the clear fluid that bathes the brain and spinal cord.
What is the life expectancy of someone with aortic stenosis?
Severe symptomatic aortic stenosis is associated with a poor prognosis, with most patients dying 2–3 years after diagnosis.
What is the life expectancy of someone with moderate aortic stenosis?
Aortic stenosis (AS): Patients with severe AS develop symptoms in 3 to 5 years. Around 75% of patients with unoperated aortic stenosis may die 3 years after the onset of symptoms.
What is the life expectancy of someone with a bicuspid aortic valve?
1 Aortic stenosis is the most common clinically relevant consequence of BAV and usually presents between 50 and 70 years of age. 2 If left untreated, severe aortic valve stenosis is associated with an annual mortality of 25% and the mean duration of survival after diagnosis is 2–3 years.
What should you avoid with a bicuspid aortic valve?
Most people with BAV can safely exercise without significant restrictions. Strenuous isometric exercise (e.g., weight-lifting, climbing steep inclines, chin-ups), should be avoided if there is severe valve disease, or moderate to severe aortic ectasia.
What medication is indicated for aortic insufficiency due to aortic stenosis?
ACE inhibitors, which can open blood vessels more fully. Medicines that tame heart rhythm problems. Beta-blockers, which slow your heart rate. Diuretics (“water pills”), which lessen the amount of fluid in your body and ease stress on your heart.
Does metoprolol help aortic stenosis?
Metoprolol Reduces Hemodynamic and Metabolic Overload in Asymptomatic Aortic Valve Stenosis Patients.
Why is nitroglycerin contraindicated in aortic stenosis?
Nitrates are contraindicated due to their potential to cause profound hypotension in aortic stenosis. Any hypertension is treated aggressively, but caution must be taken in administering beta-blockers.