Why JVP is measured in internal jugular vein
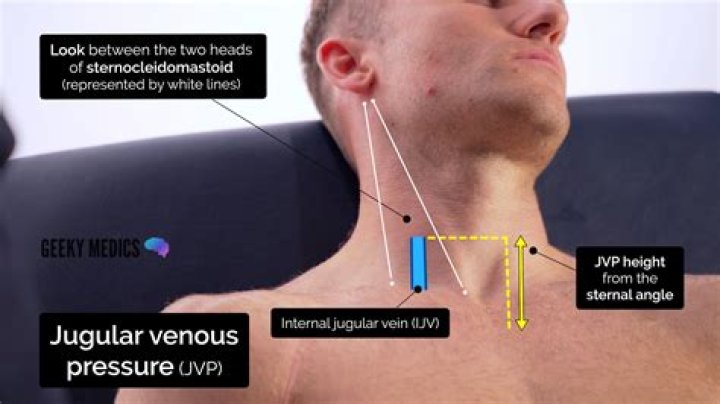
Jugular venous pressure (JVP) provides an indirect measure of central venous pressure. The internal jugular vein connects to the right atrium without any intervening valves – thus acting as a column for the blood in the right atrium.
Why is the internal jugular vein preferred to record JVP?
While both internal and external jugular veins are used to estimate the JVP, the internal jugular vein is preferred because the external jugular vein has valves and is not directly in line with the superior vena cava and right atrium.
Why is the right internal jugular vein preferred?
The right internal jugular vein is the preferred catheter location compared with the left internal jugular and subclavian vein sites; it provides a straight route to the right atrium, thereby reducing the risk of central vein stenosis. Catheters may also be placed in the femoral veins.
Is JVP internal jugular vein?
Jugular venous pressure (JVP) provides an indirect measure of central venous pressure. This is possible because the internal jugular vein (IJV) connects to the right atrium without any intervening valves, resulting in a continuous column of blood.What is the purpose of jugular vein pressure assessment?
The jugular venous exam is an important aspect of assessing a patient’s volume status, especially in patients with heart failure, liver failure and kidney failure. Both elevation of the neck veins and the variations of the neck vein waveforms share valuable information about a patient’s diagnosis.
Why is JVP elevated in heart failure?
Elevated jugular venous pressure is a manifestation of abnormal right heart dynamics, mostly commonly reflecting elevated pulmonary capillary wedge pressure from left heart failure. This usually implies fluid overload, indicating the need for diuresis.
Why does JVP decrease with inspiration?
JVP normally decreases during inspiration because the inspiratory fall in intrathoracic pressure creates a “sucking effect” on venous return. Thus, the Kussmaul sign is a true physiologic paradox. This can be explained by the inability of the right side of the heart to handle an increased venous return.
Where is the internal jugular vein?
The IJV is located between the clavicular heads of the sternocleidomastoid. It is accessed best at the apex of the triangle the muscle heads make with the clavicle (see the image below). Neck anatomy showing course of internal jugular vein (IJV).What is JVP and its clinical importance?
The jugular venous pressure (JVP, sometimes referred to as jugular venous pulse) is the indirectly observed pressure over the venous system via visualization of the internal jugular vein. It can be useful in the differentiation of different forms of heart and lung disease.
What position is best for evaluating jugular venous distention?To properly evaluate jugular venous distension, the patient must be placed at a 45-degree angle, or slightly less. Visualization of the jugular veins is best done at an oblique angle, so sit beside the patient and elevate the head of the cot into a semi-Fowler’s position.
Article first time published onCan you see the internal jugular vein?
Internal jugular veinTA24800FMA4724Anatomical terminology
Is visible JVP normal?
Normally only the a and v waves are visible. Conditions associated with an elevated JVP include congestive heart failure and fluid overload.
What is Pulsus Paradoxus?
Pulsus paradoxus is defined as a fall of systolic blood pressure of >10 mmHg during the inspiratory phase.
What is a positive HJR?
A positive HJR sign is defined by an increase in the jugular venous pressure (JVP) > 3 cm, sustained for greater than 15 seconds, and signifies that the right ventricle cannot accommodate the augmented venous return.
Why JVP is elevated in cardiac tamponade?
The decline in cardiac output leads to hypotension and cool extremities. The jugular venous pressure rises which may show as venous distension at the neck and head. Acute cardiac tamponade is usually caused by bleeding due to trauma, aortic dissection or is iatrogenic.
What is internal jugular vein?
The internal jugular vein is a paired venous structure that collects blood from the brain, superficial regions of the face, and neck, and delivers it to the right atrium. The internal jugular vein is a run-off of the sigmoid sinus.
What is IJ catheter?
It is often used for reliable venous access in ill patients. There are numerous routes of central venous access including internal jugular (IJ), subclavian and femoral. This module will focus on internal jugular central venous catheter placement.
How is jugular distension measured?
- Examine position. Head of bed elevated at 45 degree angle. …
- Identify top of venous pulsation in neck (JVP) Jugular Venous Pulsations are inward. …
- Identify the sternal angle (Angle of Louis) …
- Measure distance between top of pulsation and Sternum.
What is a finder needle?
* A finder needle is a thinner needle used for locating the vein before inserting the introducer needle. It is generally recommended for nonultrasound–guided internal jugular vein cannulation.
What is an EJ line?
[/su_tab] [su_tab title=”External Jugular Vein (EJ)”] The EJ vein is a great site for rapid IV access. It can often be accessed without ultrasound guidance and is a large vein that can often be used for medication/fluid administration and phlebotomy.
How long do IJ lines stay in?
CVLs are inserted at femoral, subclavian and internal jugular sites. The internal jugular vein is the most common site used in children when the line will be in place for longer than seven to 14 days.



